The following are just some notes to help me in future articles, that’s why I’m not emailing this out to everyone.
For a while now I’ve been thinking about latent viruses. I wrote this back in May:
My quickly sketched hypothesis is that the engineered virus compromises our immune systems, enabling the reactivation of latent viruses, which in turn play hell with our immune systems. In my case, this has resulted in muscle spasms, “electric” shocks all over my body, flashing lights in my left eye, nerve damage (hands and feet on fire with tingling), burning sensations on my face, falling over (not often), difficulty swallowing, and my main concern: problems with thinking/memory.
My doctor thought I might have MS, so I had an MRI scan. I recently got the results: I do not have any plaques on my brain. It doesn’t mean that I’m not on my way to MS, but you could speculate that about anyone, right? I’m on a waiting list to see a neurologist, but since that waiting list is just under 2 years, I think the sensible thing to do is to try and see if I can fix myself first. Incidentally, there is a connection between the Epstein-Barr Virus and MS. This brings me back to the idea about latent viruses being a possible root cause of my condition, whatever that is, and also the general rise in autoimmune issues we are observing.
I decided to ask ChatGPT about latent viruses:
ChatGPT, can you give me a list of latent viruses?
Certainly, latent viruses are a fascinating subject in virology. They are viruses that can infect a host and remain dormant for an extended period before becoming active again. During the latent phase, the virus is generally not causing symptoms, and it may be challenging to detect its presence. The ability of a virus to become latent allows it to evade the host's immune system and persist for long periods, sometimes for the lifetime of the host.
Here's a list of some viruses known to establish latency:
Herpesviruses
Herpes Simplex Virus 1 (HSV-1): Causes oral herpes but can also cause genital herpes.
Herpes Simplex Virus 2 (HSV-2): Primarily causes genital herpes.
Varicella-Zoster Virus (VZV): Causes chickenpox and shingles.
Cytomegalovirus (CMV): Can cause mononucleosis-like symptoms.
Epstein-Barr Virus (EBV): Causes infectious mononucleosis ("Mono").
Human Herpesvirus 6 (HHV-6): Associated with roseola in infants.
Human Herpesvirus 7 (HHV-7): Also associated with roseola.
Human Herpesvirus 8 (HHV-8): Associated with Kaposi's sarcoma.
Retroviruses
Human Immunodeficiency Virus (HIV): Causes AIDS.
Papillomaviruses
Human Papillomavirus (HPV): Causes warts and is linked to certain cancers.
Polyomaviruses
JC Virus: Can cause progressive multifocal leukoencephalopathy (PML) in immunocompromised individuals.
BK Virus: Generally asymptomatic but can cause problems in immunocompromised individuals.
Hepadnaviruses
Hepatitis B Virus (HBV): Causes hepatitis B, can lead to liver cancer.
Others
Adenovirus: Usually causes mild respiratory infections but can become latent in lymphoid tissue.
It's important to note that the mechanisms by which these viruses establish and maintain latency can vary widely and are the subject of ongoing research. The list is not exhaustive, and the understanding of viral latency is continually evolving.
Is it possible to entirely remove a latent virus from your body?
The question of whether it's possible to entirely remove a latent virus from the body is a complex and nuanced one. The general consensus in the scientific community is that completely eradicating latent viruses is extremely challenging, if not currently impossible, for most types of latent viruses.
Why is it Difficult?
Cellular Integration: Some latent viruses, like HIV, integrate their genetic material into the host's genome. This makes it difficult to target the virus without damaging the host cell.
Immune Evasion: During latency, many viruses downregulate the expression of viral proteins, making it difficult for the immune system to recognize and eliminate infected cells.
Anatomical Reservoirs: Some viruses hide in specific tissues where drug penetration is poor or where the immune system has limited access.
Reactivation: Even if a treatment reduces the viral load to undetectable levels, it doesn't guarantee that the virus has been entirely eradicated. Some cells harboring the virus may reactivate at a later time.
Current Treatments and Limitations
Antiviral Medications: These can control the symptoms and reduce the viral load but generally do not eliminate the virus entirely.
Immunotherapies: These aim to boost the immune system to recognize and eliminate infected cells but have shown limited success in completely eradicating latent viruses.
Gene Editing: Technologies like CRISPR have been explored for excising viral genomes from host cells, but this is still experimental and comes with ethical and safety concerns.
Alternative Perspectives
While mainstream medicine has its viewpoints, it's worth noting that there are alternative theories and experimental treatments aiming to eradicate latent viruses. However, these are often not widely accepted and may lack robust clinical evidence. Therefore, skepticism and critical evaluation are essential when considering such options.
What are some alternative theories and experimental treatments aiming to eradicate latent viruses?
The quest to eradicate latent viruses has led to a variety of alternative theories and experimental treatments, some of which exist on the fringes of mainstream medicine.
Alternative Theories
Viral Persistence: Some theories suggest that latent viruses may not be entirely "dormant" but could be actively modulating the immune system in subtle ways. This opens the door for treatments aimed at "unmasking" these viruses to the immune system.
Holistic Approaches: Theories that consider the body as an interconnected system suggest that improving overall health and reducing stress may help the body naturally clear latent viruses.
Co-Infection Synergies: Some theories propose that latent viruses may interact with other pathogens in the body, and that targeting these co-infections may help in eradicating the latent virus.
Experimental Treatments
Gene Therapy: Experimental approaches using CRISPR or other gene-editing technologies aim to excise the viral genome from host cells.
Immune Modulation: Treatments like low-dose naltrexone (LDN) aim to modulate the immune system to better target latent viruses.
Peptide Therapies: Some experimental treatments use peptides to target specific viral proteins and disrupt the virus's ability to maintain latency.
Nutraceuticals: Compounds like quercetin and resveratrol are being studied for their potential antiviral properties, including against latent viruses.
Ozone Therapy: This involves the introduction of ozone into the body through various methods, purportedly to improve oxygenation and immune function. However, the evidence supporting its efficacy is limited.
Hyperthermia: The idea here is to raise the body's temperature to create an environment where the virus is less stable, although this is a risky approach.
Phage Therapy: Using bacteriophages to target bacteria that may be harboring latent viruses is another experimental approach.
Stem Cell Therapy: Some experimental treatments are exploring the use of stem cells to regenerate tissues damaged by latent viruses, although this wouldn't necessarily eradicate the virus.
Given the complexity of viral latency and the limitations of current treatments, alternative theories and experimental approaches offer intriguing possibilities.
Please make a list of the nutraceutical attempts to rid the body of latent viruses, and how they are supposed to work.
Nutraceuticals are food-derived substances that are used in the form of supplements or functional foods to provide health benefits. While some people turn to nutraceuticals in an attempt to manage or even eradicate latent viral infections, it's important to approach these options with a critical mindset. The efficacy of nutraceuticals in eradicating latent viruses is not well-supported by robust scientific evidence, and their proposed mechanisms of action are often based on limited studies or theoretical considerations.
List of Nutraceuticals and Their Proposed Mechanisms
(this is the list suggested by ChatGPT, with links to papers suggested by ChatGPT unless otherwise stated).
Lysine
Proposed Mechanism: Believed to inhibit the replication of herpes simplex virus by competing with arginine, an amino acid that the virus needs to replicate.
The observed studies have shown that the usual antiviral therapies are not able to interfere with the viruses in their latent state; however, they can interfere with the adhesion and fusion of viral particles or the production of proteins, which play an important role in viral epidemiology and control, particularly in the initial moment and in reactivation. Lysine is an amino acid that can interfere mainly in the formation of capsid proteins and DNA by a competitive antagonism with amino acid arginine, which is an essential amino acid for some viruses, and also by promoting the increase of arginase, increasing the catabolism of arginine. Although there is evidence of the importance of L-lysine in viral control, more studies are needed, with a view to new antiviral therapies.
Lysine therapy has long been recommended against HSV infection because it can suppress viral replication and inhibit virus yield [23,26,27,28,38]. HSV growth in both cell and tissue cultures that were supplemented with arginine was suppressed upon the addition of lysine [22]. A trial conducted on subjects with recurrent HSV infection also proved the efficacy of lysine treatment against HSV when the lysine group reported less recurrence, shortened healing time, and milder symptoms during six months of taking L-lysine monohydrochloride tablets while avoiding arginine-rich foods. [27]. These are just a few of the studies proving the efficacy of lysine as a prophylactic agent for HSV infection. Considering the prophylactic effects of lysine, a recent observational study was conducted using lysine therapy as prophylaxis for SARS-CoV-2 infection.
Among 30 medical professionals with daily face-to-face exposure to COVID-19 patients, all remain negative of the virus after taking 2000 mg lysine daily with required dietary restrictions (no caffeine, marijuana and arginine-rich foods) for 3 months, as compared to an average of two employees being infected every month prior to the study and to a public health department with similar capacity as their control group [39]. Our study validates that lysine has protective effects against SARS-CoV-2 and IAV infection. Thus, lysine supplementation may be considered as prophylaxis and therapeutic tool against these viruses.
Previous studies on HSV and IAV infection demonstrated that arginine can promote virus infection and replication [20,22,38]. In agreement, our data showed that pre-treatment of Arg-ester had a pronounced augmenting effect on both SARS-CoV-2 and IAV infection (Figure 2A and Figure 4). Cellular protease TMPRSS2 promotes SARS-CoV entry by cleaving S protein to activate it for membrane fusion and by cleaving ACE2 that leads to increased virus uptake [40]. As observed in Figure 3A, Arg-ester treatment caused the formation of a smaller ACE2, supposed to be the cleavage of ACE2. These findings suggest that Arg-ester may promote SARS-CoV-2 infection by inducing ACE2 cleavage.
Specifically, bioinformatics and biochemical experiments showed that by interacting with 40S ribosomal subunit, the lysine located at amino acid 164 (K164) was the key residue that enabled SARS-CoV-2 nsp1 to suppress host gene expression. Furthermore, as an inhibitor of host-protein expression, SARS-CoV-2 nsp1 contributed to cell-cycle arrest in G0/G1 phase, which might provide a favourable environment for virus production. Taken together, this research uncovered the detailed mechanism by which SARS-CoV-2 nsp1 K164 inhibited host gene expression, laying the foundation for the development of attenuated vaccines based on nsp1 modification.
Quercetin
Proposed Mechanism: Has anti-inflammatory and antiviral properties; thought to inhibit viral replication and modulate immune response.
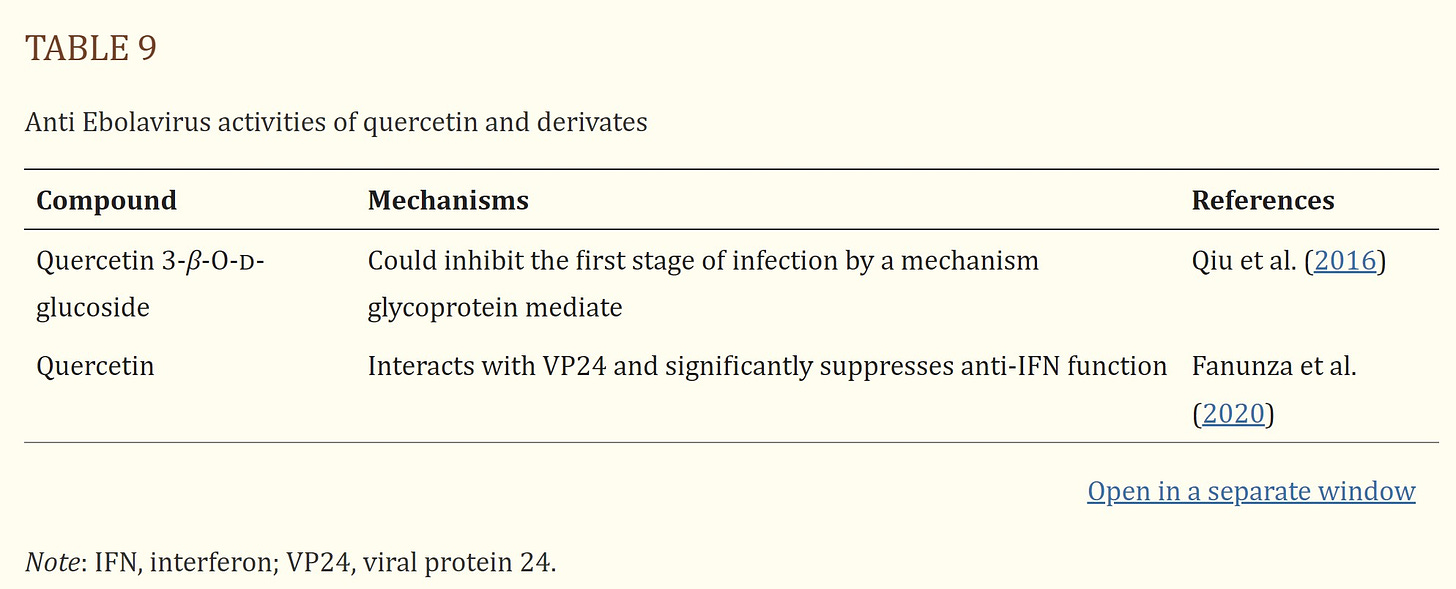
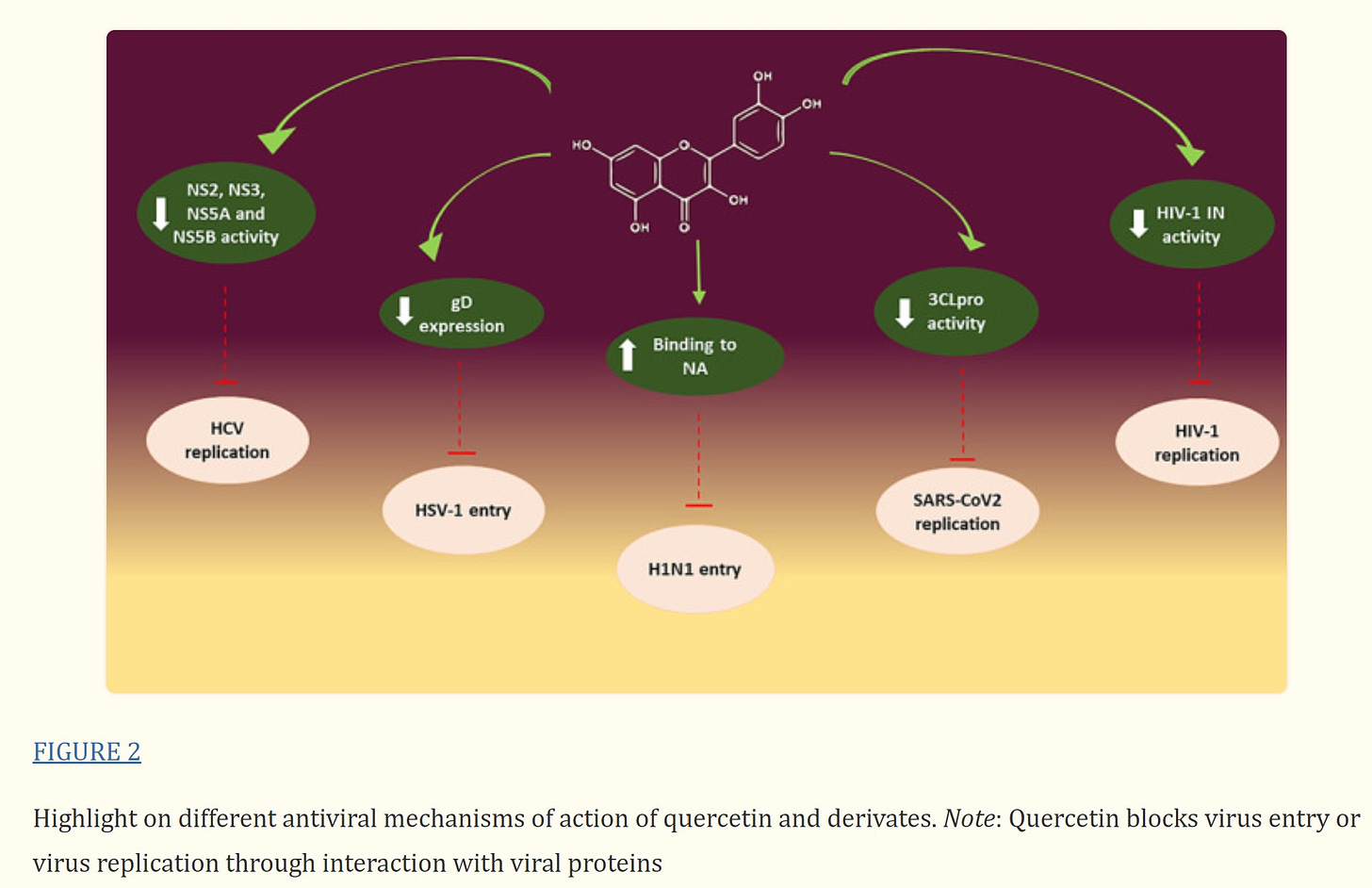
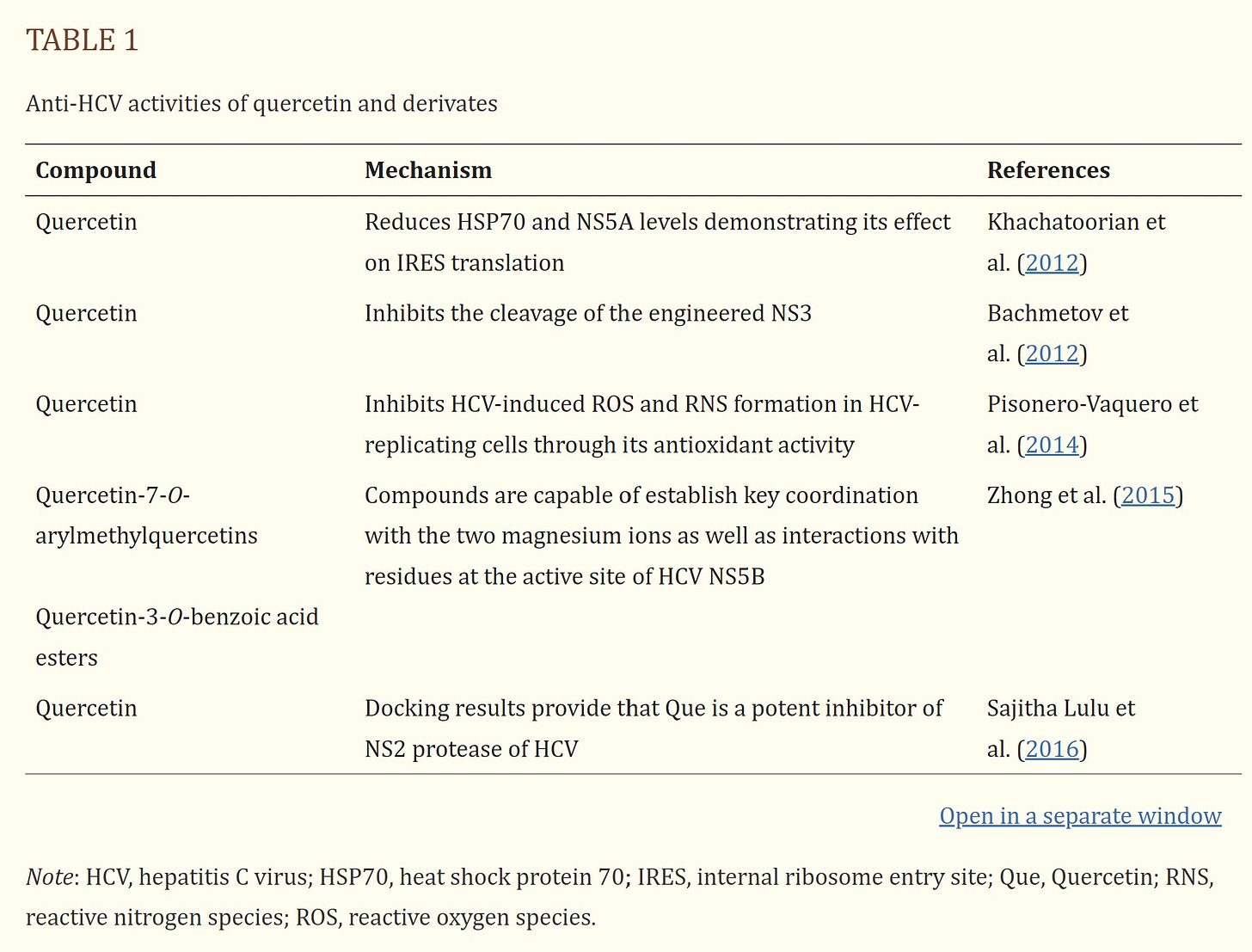
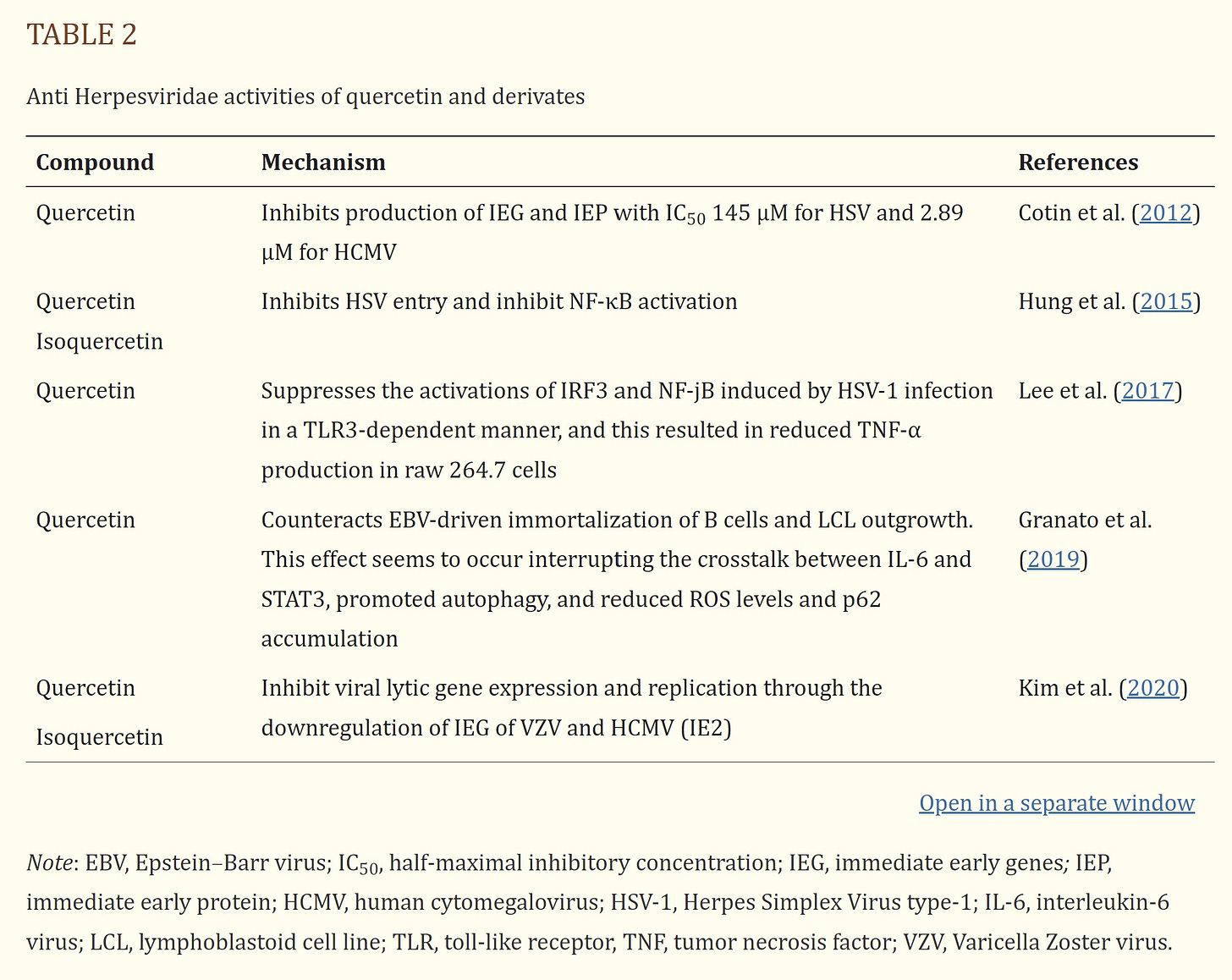
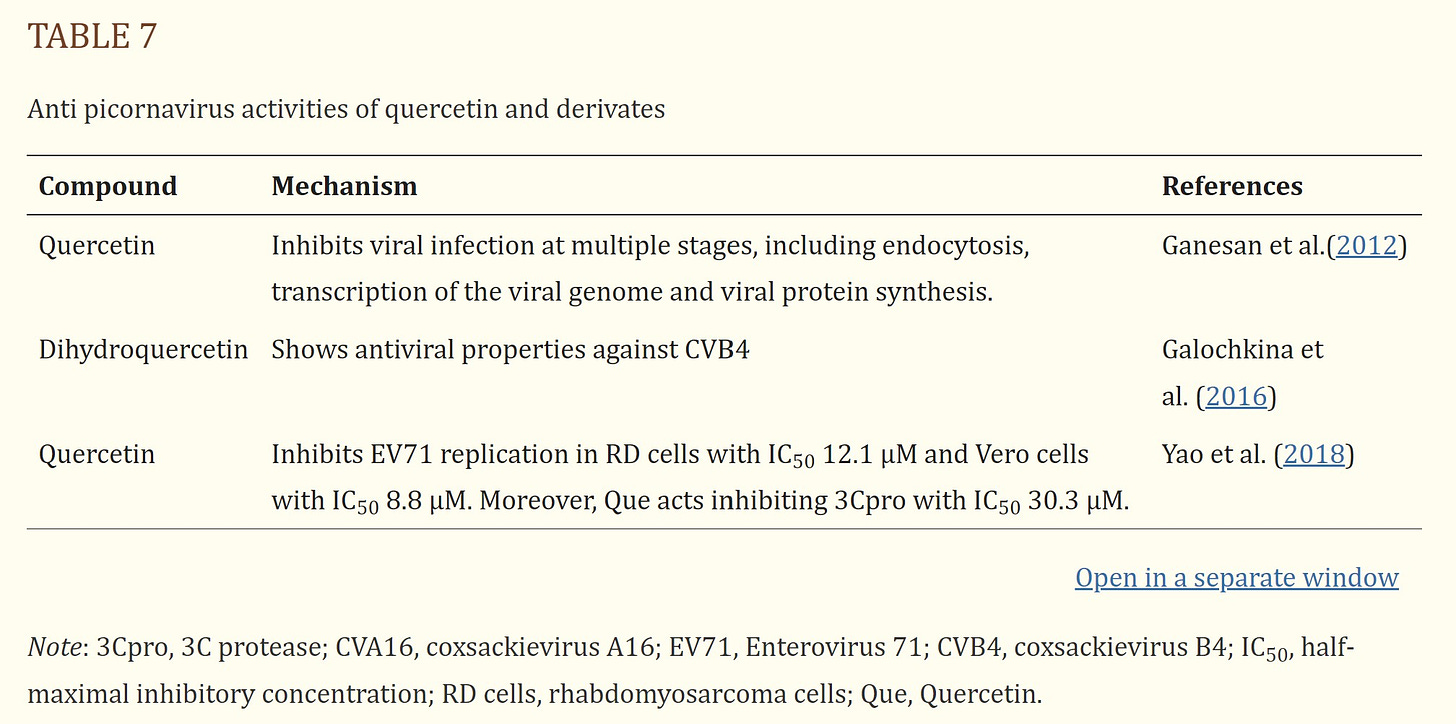
Quercetin and its derivatives are naturally occurring phytochemicals with promising bioactive effects such as immunoprotective, antiinflammatory, and antiviral effects. In this review the antiviral activity of quercetin and its derivates against potential human viruses was collected. Quercetin showed a potent antiviral activity in vitro and the different mechanisms of action are reported in Figure 2.
Particularly, quercetin seems to block virus entry by interacting with membrane glycoproteins such as gD of HSV and NA of H1N1. Moreover, molecular docking studies have shown that quercetin and its derivatives could interact with specific proteases essential for viral replication, such as NS2, NS3, and NS5A of HCV, integrase and TOP2 of HIV, Mpro of Coronaviridae, and 3Cpro of Enterovirus.
All these studies shown how the quercetin and its derivates have a wide spectrum of antiviral activities and a better understanding of quercetin's mechanistic properties could help in the rational design of more potent or bioavailable flavonol‐type compounds.
In such scenario, the phytochemical agents that have demonstrated immune-modulatory, anti-viral, anti-inflammatory and antioxidant properties, along with an excellent safety profile, could be used to boost the body immune system, to reduce excessive inflammation, to inhibit viral replications and to help in preventing the COVID-19 disease development and progression. Quercetin is a phytochemical and a dietary supplement that has widely demonstrated these properties. Particularly, its antioxidant and anti-inflammatory properties seem to be closely related to its effective role against a variety of conditions related to inflammation, including viral infections, respiratory diseases, allergies, asthma, hay fever, arthritis, atherosclerosis, hypercholesterolemia, heart disease and circulatory disorders, insulin resistance and diabetes, eye-related disorders (including cataracts), stomach ulcers, cognitive impairment, gout, cancer, chronic fatigue syndrome, inflammation of the prostate, bladder, and ovaries, chronic infections of the prostate, skin disorders, including dermatitis and hives.14 Besides the “historical” pharmaco-clinical findings, the volume of data produced in the last 15 months for quercetin suggesting that this polyphenol could be a potential candidate for COVID-19, strongly prompted us to carried out a clinical study aimed to highlight its possible role within the context of this disease. Quercetin is a lipophilic compound, so it is assumed that it can cross the intestinal membranes by simple diffusion, and theoretically, this absorption is better than its glycoside forms which reach the intestines without degradation. Nevertheless, human data describe a very low oral absorption for quercetin. Due to the quercetin poor pharmacokinetics profile, it has been decided to use a lecithin delivery system form of quercetin (QP), described to be up to 20-folds more bioavailable than a not-formulated one.17 According to the kinetic parameters obtained in humans, the bioavailability rate of quercetin after the oral use of the phytosome form can be considered very far from the one considered toxic and obtained after intravenous injection in subject with cancer.20 We have then carried out a prospective, randomized, controlled and open-label study to evaluate the anti-COVID-19 effects of this orally bioavailable form of quercetin on symptomatic outpatients. According to the results of this clinical research, the add-on therapy with QP has significantly reduced the need (−68.2%) and the length (−76.8%) of hospitalization, the need of non-invasive oxygen therapy (−93.3%), the progression to intensive care units (none versus 8 subjects) and the number of deaths (none versus 3 subjects). Globally considered, the effect of QP seems to have a strong impact not only considering the difference in terms of admission to ICU and in terms of fatal outcome, but particularly considering the difference in terms of days of hospitalization. The days spent by subjects whose disease progressed and needed hospitalization were 131 for SC group and 11 for the QP one. This difference means that using QP as add-on therapy to standard care has reduced by 91.6% the days of hospitalization. Along with these results, QP not only has shown to be well tolerated and devoid of peculiar side effects, but was also reported by subjects to be beneficial against chronic fatigue and tiredness, and appetite lost, being this last two aspects commonly described as COVID-19 possibly invalidating related sequelae
There are many studies claiming Quercetin helps with SARS-COV-2:
Resveratrol
Proposed Mechanism: Known for its antioxidant properties, it's also believed to inhibit viral replication and modulate the immune system.
Resveratrol is a naturally appearing polyphenol (trans-3,4′,5-trihydroxystibene), mainly sourced from grape skin and red wine as well as medicinal plants e.g., Japanese knotweed, that has been used over many years in different chronic diseases for its antioxidant, anti-inflammatory and anti-tumorigenic properties [19]. There is growing evidence that the redox status of cells plays an important role in viral infections. RNA and DNA viruses can decrease glutathione levels and glutathione supplementation can inhibit viral replication [20], [21]. Resveratrol inhibits the influenza virus replication - it was thought that this was due to resveratrol’s influence on cellular redox status via glutathione. However, this inhibition was demonstrated not to be directly associated to glutathione mediated antioxidant activity, but by inhibiting nuclear-cytoplasmic translocation of viral ribonucleoproteins and reducing the expression of late viral proteins associated with the inhibition of protein kinase C [20]. Resveratrol derivatives have been tested in vitro with some success on viral particle infectivity for the possible development of new influenza treatments [22]. Combinations such as resveratrol with N-acetylcysteine or glutathione, which have both antioxidant and antiviral effects, inhibits the proliferation of influenza virus and are of specific interest for serious influenza-associated complications [23].
Resveratrol has also been found to be a moderate inhibitor of the N1L protein which is a virulence factor in viral infections such as smallpox [24]. Furthermore, resveratrol has been found to act synergistically with decitabine to inhibit human immunodeficiency virus type 1 (HIV-1) infectivity without a corresponding increase in cellular toxicity [25]. It also inhibited drug-resistant HIV-1 strains with reverse transcriptase containing the M184V mutation [26]. Resveratrol had an even greater antiviral activity against the “more difficult to treat” human immunodeficiency virus type 2 (HIV-2) than HIV-1 and its antiviral activity appeared to be selective for the reverse transcription phase of virus replication [27]. A novel synthetic resveratrol derivative namely 3,3′,4,4′,5,5′-hexahydroxy-trans-stilbene has also been developed and demonstrated to have potent anti-HIV 1 activity – the authors suggested that this derivative may have a potentially different mechanism of action to current anti-HIV-1 drugs including entry inhibitors [28].
It appears that resveratrol has inhibitory activity against various viral enzymes, for example it acts as an inhibitor of ribonucleotide reductase and antiretroviral synergy was described between resveratrol and 5-azacytidine, a ribonucleoside analog, which is of significance in HIV-1 treatment [29]. Resveratrol’s antiviral activity against the herpes simplex virus appears to be via the same mechanism, namely inhibition of ribonucleotide reductase, impairing the expression of viral proteins [30]. Additionally, a resveratrol tetramer also showed high potency as inhibitor of the hepatitis C virus helicase [31]. Resveratrol also demonstrated a potent inhibitory effect on pseudorabies virus - a major devastating disease in the swine industry, due to its inhibition of nuclear factor kappa B (NF-κB) activation and NF-κB-dependent gene expression via its inhibitory effect on ikappaB (IκB) kinase degradation [32].
In vitro testing showed that resveratrol also partially inhibited the replication of respiratory syncytial virus - one of the most common pathogens of lower respiratory diseases in children, as well as decreased interleukin-6 production [33]. Resveratrol was also tested in combination with beta-glucan for the treatment of pediatric recurrent respiratory infections. In a global real-life randomized study with 82 children, an aerosolized solution of resveratrol plus carboxymethyl-beta-glucan significantly reduced nasal symptoms, cough, and fever, as well as reducing the need for medication and medical visits [34]. This combination was furthermore tested in vitro for its effect on human rhinovirus replication (HRV) and was found effective to inhibit the production of several HRV-induced inflammatory mediators in the nasal epithelia, possibly due to resveratrol’s ability to suppress viral replication [35].
Another postulated mechanism of action of resveratrol is to change cellular metabolism and signal transduction pathways by affecting enzymes, such as adenosine monophosphate kinase and the serine/threonine protein kinase that is the mechanistic target of rapamycin (mTOR), since these pathways influence immune function and cellular inflammation status [36]. Overall, the antiviral mechanisms of resveratrol in human and animal viral infections appear to include inhibition of viral replication, protein synthesis, inhibition of transcription and signaling pathways, as well as viral related gene expressions [37], [38]. Resveratrol could also, by its effect of restoring glutathione levels, inhibit monocyte to macrophage differentiation and inflammation [39].
In many countries patients do not have access to current or new antiviral treatments and are often only treated symptomatically or sometimes with additional nutritional support in the form of vitamins and minerals i.e., vitamin D and zinc. In these cases, resveratrol can prove a valuable addition to the supportive treatment regime, whether alone or as an adjuvant supportive antiviral treatment. As discussed before, not only does resveratrol act as an antiviral but can also play a role in stimulation of the immune system and down regulation of the pro-inflammatory cytokine release, as well as reducing lung injury by reducing oxidative stress
Anti-viral effects
RV has demonstrated antiviral effects in a variety of animal and human diseases2. Specific to CoV, in vitro studies demonstrate that RV inhibits MERS-CoV infection by decreasing nucleocapsid protein expression resulting in reduced viral production and increased cell survival33. Starting at the first steps in the infection, in silico modeling suggests that RV would interfere with the binding of CoV spike protein to the ACE2 receptor (Fig. 1)4,5. In silico analysis also suggests that RV would inhibit COVID-19 RNA Dependent Polymerase and Papain-like Protease (PLpro) (Fig. 1) which could explain the inhibition of nucleocapsid protein described by Lin et al.6,10,33. In silico analysis also demonstrates potential inhibition of the coronavirus main proteinase (Mpro) which would be an additional mechanism of inhibiting viral replication7.
Anti-inflammatory effects
COVID-19 is associated with the potential for excessive inflammation. Coronavirus has been shown to activate Toll-Like Receptor 4, increase pro-inflammatory cytokines IL-1, IL-6, CCL5 (RANTES) and TNF-α leading to an unbalanced inflammatory response and damaging inflammation34,35,36,37. In contrast, RV has been shown to reduce inflammation via a variety of mechanisms (Fig. 1)11,12,13,38. RV has been demonstrated to inhibit TLR4 activation, decreasing the release of inflammatory cytokines in the macrophages of patients with COPD, and inhibit the proinflammatory transcription factor NF-κB14,19,39. RV has also demonstrated inhibition of pro-inflammatory Th17 helper T-cells (Fig. 1)20. Inhibition of NF-κB has been shown to increase survival in a mouse model of SARS-COV140.
The anti-inflammatory effects of RV might be beneficial in mitigating the cytokine storm that is associated with ARDS and the high mortality of COVID-1925. A mouse model of cytokine storm showed a 100% mortality reduced to 0% in RV treated mice with minimal lung injury in the treated group41. RV has demonstrated protective effects in lipopolysaccharide induced lung injury, a mouse model of ARDS42,43. The proposed mechanism is RV’s inhibition of NLRP3 inflammasomes42. Inhibition of NLRP3 inflammasomes in another proposed therapeutic target in COVID-1944.
Antioxidant effects
Depletion of the endogenous antioxidant glutathione has been attributed to poor outcomes and death in patient with COVID-19 (Fig. 1)21. The use of antioxidants has been proposed in the treatment of COVID-1945. RV’s antioxidant properties as well as its ability to induce glutathione synthesis might provide additional outcome benefits22.
Animal models of viral infections
As the above discussion regarding RV’s effects are largely based on in vitro models of disease, there is always a concern regarding whether in vitro models will translate into in vivo efficacy. Multiple animal studies have shown that RV does improve outcomes in animal models of viral infections. A porcine model of pseudorabies virus, a respiratory illness, shows that piglets inoculated with the virus had no mortality compared to a 40% mortality in the untreated group. Specifically, that study showed alveolar destruction in the untreated group vs mild lung injury in the RV treated group. The proposed mechanism is inhibition of IκB kinase by RV46. It is notable that a drug prediction analysis of SARS-CoV-2 suggests that IκB kinase inhibition is a potential target for COVID-1947. Similarly, a murine model of H1N1 influenza showed a 60% survival rate in RV treated mice compared to 20% in placebo treated mice48. In Respiratory Syncytial Virus (RSV) infected mice, RV treated mice showed significantly less lung damage compared to untreated mice49.
Vitamin D3
Vitamin D3 was included in the treatment protocol as an adjunct to RV based upon prior research showing that it has synergistic anti-inflammatory effects, inhibiting IL-6 and TNF-α11. Both treatment arms received a single 100,000 IU dose of D3 to quickly assure adequate serum concentrations of D3, as well as to potentially remove vitamin D deficiency as a confounding variable, noting that multiple publications raised concerns that vitamin D deficiency might be associated with worse outcomes in COVID-1950,51,52. The empiric use of vitamin D3 could lower the overall incidence of adverse outcomes in both groups in this study.
This proof-of-concept study, along with the wealth of other resveratrol pre-clinical research, supports further investigation resveratrol as a potential treatment of COVID-19 and possibly other viral respiratory infections (including influenza, Respiratory Syncytial Virus, and Human Rhinovirus)70. If the magnitude of the effect of this small study was representative of a larger trial, the number needed to treat to prevent ER visits or hospitalization would compare favorably against currently available (i.e., monoclonal antibody therapy) outpatient treatments.
The antiviral mechanisms and effects of RSV have been widely studied in a number of viruses which include influenza virus, hepatitis C virus [4], respiratory syncytial virus [5–9], varicella zoster virus [10], Epstein-Barr virus [11, 12], herpes simplex virus [13–16], human immunodeficiency virus [17, 18], African swine fever virus, enterovirus, human metapneumonia virus, and duck enteritis virus and in multiple sclerosis, whose animal models can be induced by viral infection. In almost all of these studies, RSV showed remarkable recession of the viral infection with the exception of multiple sclerosis and hepatitis C, where disease progression was worsened following administration of RSV [4, 19].
In influenza virus infection, RSV was shown to actively block nuclear-cytoplasmic translocation of viral ribonucleoproteins in MDCK cells, thus decreasing the expression of late viral proteins related to inhibition of protein kinase C associated pathways. This activity was also found to be unassociated with glutathione-mediated antioxidant activity of the compound [30].
In Epstein-Barr virus (EBV) infection, RSV showed an enhanced inhibitory effect on EBV early antigen induction using Raji cells. It was also shown to reduce papilloma production in mouse by 60% after 20 weeks of inoculation [31]. In another study, RSV was shown to dose-dependently inhibit EBV lytic cycle by inhibition of transcription genes and proteins, Rta, Zta, and diffused early antigen (EA-D), as well as inhibiting the activity of EBV immediate-early protein: BRLF1 and BZLF1 promoters. This effect was seen to reduce virion production [12]. Similarly, another in vitro study confirmed the previous finding that RSV does inhibit lytic gene expression and viral particle production in a dose-dependent manner. Here its main antiviral mechanism was associated with inhibition of protein synthesis, reduction in ROS production, and inhibition of transcription factors NF-κβ and AP1 [32]. Since EBV is one of the most renowned oncogenic viruses, it is pertinent to study the role of EBV in cellular transformation and cancer progression. RSV was thus shown to prevent transformation of EBV in human B-cells through downregulation of antiapoptotic proteins: Mc1 and survivin. This was also linked to suppression of EBV induced signaling of NF-κβ and STAT-3, as well as miR-155 and miR-34a in EBV infected cells [11].
RSV was shown to inhibit the replication of herpes simplex virus-1 and herpes simplex virus-2 (HSV-1 and HSV-2) in a dose-dependent and reversible way. In this study, the authors observed a reduction in virus yield as a result of inhibition of an early event in the replication cycle: decreased production of early viral protein ICP-4. RSV also delayed interphase stage of the cell cycle and prevented virus reactivation in neuron cells that were latently infected [15]. In another study by the author using nude mice, topical application of 12.5% and 15% resveratrol ointment suppressed the development of cutaneous lesions in abraded skin infected with HSV-1 [16]. Similarly, application of 19% RSV cream on the vagina of mouse infected with HSV-2 and HSV-1 completely prevented the development of vaginal lesions, while the mortality rate was 3% as compared to the placebo group where mortality rate was 37% [14]. These remarkable effects of RSV on HSV-1 and HSV-2 infections were reported to be due to the promotion of a rapid and sustained release of ROS, which resulted in the inhibition of NF-κβ and extracellular signal-regulated kinases/mitogen-activated protein kinases (Erk/MAPK), as well as a blockade in the expression of immediate-early, early, and late HSV genes and viral DNA synthesis [13, 33].
Respiratory syncytial virus (RPSV) infection is one of the most important viral diseases of the respiratory system affecting humans and it has no specific treatment. Administration of RSV in mice infected with RPSV reduced the accompanying inflammation and levels of interferon-gamma (IFN-γ). The mechanism here was attributed to control of toll-like receptor 3 expression, inhibition of toll/IL-1R domain-containing adaptor inducing IFN (TRIF) signaling, and induction of muscarinic 2 receptor (M2R) [9]. In an in vitro study, RSV treatment in epithelial cells inoculated with RPSV resulted in decreased production of interleukin- (IL-) 6 and a partial reduction in viral replication. There was also an inhibition of viral induced toll-like receptor domain and TANK binding kinase 1 (TBK1) protein expression [7]. RSV treatment of mice infected with RPSV was shown to increase sterile-α- and armadillo motif-containing protein (SARM) expression and decrease matrix metalloproteinase 12 (MMP-12) and TIR-domain-containing adapter-inducing interferon-β (TRIF) expression; these in turn decreased IFN-γ expression and airway inflammation and hyperresponsiveness (AHR) [6, 34]. In a related study, RPSV infected mice treated with RSV also showed decreased levels of inflammatory cells and AHR. However, while RSV was able to drastically reduce the levels of nerve growth factor (NGF) after 21 days of infection, the level of brain derived neurotrophic factor (BDNF) was not significantly affected in both the treated and untreated groups [9]. Combination of RSV and baicalin (a flavonoid found in numerous species of Scutellaria) joint enema was shown to increase the levels of tumor necrosis factor-alpha (TNF-α), IFN-γ, and IL-2 in mice infected with RPSV, which is believed to be among its antiviral mechanisms [5].
In the treatment of HIV-1, a combination of RSV and decitabine (a nucleoside metabolic disorder used in the treatment of myelodysplastic syndromes) was found to be more potent than RSV alone as an anti-HIV-1 drug. However, the research also reported 15 other derivatives of RSV that were more potent as an anti-HIV-1 drug [17]. Inhibition of replication of the HIV molecular clone NL4-3 containing the mutant M184V reverse transcriptase (RT) by RSV (5 μM) was reported to be associated with inhibition DNA synthesis during the reverse transcription step of the HIV life cycle. This fact was proven when administration of RSV to NL4-3 clones without the mutant M184V RT failed to inhibit viral DNA synthesis [18].
Other viruses that were inhibited by RSV include varicella zoster, which was dose-dependently and reversibly inhibited in MRC-5 cells when added to culture within the first 30 hours of infection. Here, RSV was shown to decrease the synthesis of intermediate early protein (IE 62) [10]. Enterovirus 71 (EV 71) was also susceptible to RSV treatment as the compound effectively inhibited the synthesis of its viral protein 1 (VP1) and phosphorylation of proinflammatory cytokines (IKKα, IKKβ, IKKγ, IKBα, NF-κβ p50, and NF-κβ p65) in rhabdosarcoma cell line. Secretion of IL-6 and TNF-α was also inhibited in the infected cells by RSV [35].
Duck viral enteritis (DVE) also known as duck herpes viral enteritis or duck plague is a highly fatal disease of ducks and ducklings caused by the duck enteritis virus (DEV), a herpesvirus [43, 44]. In DVE, viral replication was impaired by RSV via suppression of nucleic acid replication and suppression of viral capsid formation in vitro. Production of viral protein was also suppressed within the first 24 hours following infection [36]. RSV in combination with a bioflavonoid, quercetin, was shown to reduce cellular oxidative damage and secretion of proinflammatory mediators (IL-1α, IL-6, and TNF-α) and chemokines (CXCL10 and CCL4), through suppression of NF-κβ and interferon regulating factor (IRF-3), as well as viral replication in human metapneumonia (hMPV) virus infection. However, RSV did not affect viral gene transcription and protein synthesis [37]. African swine fever virus (ASFV) causes an acute hemorrhagic disease in pigs that results in up to 100% mortality. Resveratrol and oxyresveratrol (a hydroxylated analog of resveratrol) were also found to have a dose-dependent effect on African swine fever virus in vitro. This was achieved through inhibition of early and late viral protein synthesis, reduced viral DNA replication, and virion formation. Hence a 98–100% reduction in viral titers was observed [38]. In human rhinovirus (HRV) infection of HeLa and nasal epithelial cells, RSV was found to exhibit a high dose-dependent antiviral activity against the virus, which was achieved through reversion of HRV-induced expression of ICAM-1. In addition, reduction in the secretion of IL-6, IL-8, and RANTES was also observed [39]. In an antiviral study of resveratrol on cytomegalovirus infection of human embryonic lung fibroblast (HEL 299), RSV prevented the synthesis of viral proteins and also inhibited virus induced activation of epidermal growth factor and phosphatidylinositol-3-kinase signal transduction. Furthermore, transcription factors of NF-κβ and Sp1 were also inhibited. These mechanisms were observed to decrease the overall replication of the virus [40].
In a study conducted by Nakamura et al. [4], RSV was found to dose-dependently enhance viral RNA replication in hepatitis C virus infection in vitro. Interestingly, RSV was also reported to reverse the antiviral effects of ribavirin and interferon on HCV RNA replication and was considered nontherapeutic in the treatment of HCV infection [4]. Similarly, RSV was also found to exacerbate the clinical and histological signs of viral model of multiple sclerosis (MS), induced by Theiler's murine encephalomyelitis virus (TMEV), which belongs to the Picornaviridae [19]. Sato et al. also showed that RSV also exacerbated an autoimmune model for MS, experimental autoimmune encephalomyelitis (EAE). However, such studies are few and there are more studies highlighting the beneficial effects of RSV against viral infections, rather than its deleterious exacerbatory effects.
Curcumin
Proposed Mechanism: Has anti-inflammatory properties and is thought to inhibit viral entry into cells and viral replication.
Despite promise as an antimicrobial agent, curcumin has several limitations. Curcumin is practically insoluble in water, with low in vivo bioavailability. As little as 1% of administered curcumin is absorbed by the body.
Perhaps the largest body of work on the anti-viral properties of curcumin pertain to its efficacy against HIV. Indeed, curcumin can impact HIV function at several different stages of the virus lifecycle.
Mounce et al. [14] compared the efficacy of curcumin and several curcumin analogues against Zika (ZIKV), chikungunya virus (CHIKV) and vesicular stomatitis virus (VSV), all enveloped viruses, as well as Coxsackie B3 virus (CVB3), a non-enveloped virus. Direct incubation of ZIKV in 10 µM to 1 mM of curcumin, bisdemethoxycurcumin, demethoxycurcumin or the synthetic curcumin structural analogue EF-24 and derivative FLLL31 (originally synthesized by Adams et al. [48] and Lin et al. [49], respectively), resulted in a dose- and time-dependent decrease in subsequent virus infection, suggesting these drugs have a direct ability to inactivate virus or inhibit cell attachment.
In addition to evaluating curcumin against ZIKV, Gao et al. [15] also investigated the same selection of compounds against dengue virus (DENV). Curcumin reduced plaque formation of all four strains (DENV-1-4, IC50 of 9.37, 3.07, 2.09, and 4.83 µM, respectively) examined in LLC-MK2 cells while showing limited toxicity (CC50 of 59.42 µM) [15]. Though the mechanism of inhibition was not addressed, an earlier study demonstrated that curcumin likely inhibits DENV-2 indirectly through impact on cellular systems rather than directly on viral functions [51].
Curcumin is also a potent inhibitor of IAV, and likely exerts its effect at multiple different stages of the virus lifecycle. Incubation of IAV with curcumin results in reduced infectivity, possibly due to the ability of curcumin to interfere with viral haemagglutinin activity [19,36]. Curcumin also inhibits NF-κB signalling, which is required for IAV replication [52]. Time-of-addition experiments showed that addition of curcumin as late as 5 hpi reduced plaque formation (EC50 of ~58 µM), suggesting curcumin interferes with an early stage of virus gene expression or replication [19]. Additionally, curcumin inhibited several IAV-induced toll-like receptor (TLR) signalling pathways and proteins, which are normally required for efficient virus internalization and/or replication, including TLR2/4/7, MyD88, TRIF, and TRAF6. Indeed, treatment of cells with agonists for TLR2/4, p38/JNK MAPK or NF-κB were able to circumvent the replication block imposed by curcumin [19]. Importantly, curcumin treatment by oral gavage (50 and 150 mg/kg) reduced IAV replication and lung injury in an in vivo animal model [19], clearly illustrating that curcumin can provide a therapeutic benefit to combat infection and virus-induced disease. This latter observation was supported by a study by Han et al. [53], who demonstrated that mice infected with the IAV strain PR8 and fed 30 or 100 mg/kg of curcumin had increased survival, reduced bodyweight loss, and lower IAV burden in lung tissues as determined by immunohistochemistry. Bronchoalveolar lavage (BAL) fluid and lung tissues from infected, curcumin-treated mice had lower levels of monocyte chemoattractant protein-1 (MCP-1) and tumour necrosis factor-alpha (TNFα) compared to untreated mice, suggesting reduced inflammation. Similarly, bone marrow-derived macrophages (BMDM cells) isolated from mice and infected with PR8 produced lower levels of inflammatory cytokines IL-6, TNF-α and MCP-1 following treatment with curcumin [53]. These results indicate that curcumin is not only capable of inhibiting IAV replication, but also attenuates IAV-induced lung disease, likely through inhibition of NF-κB signaling leading to reduced secretion of inflammatory cytokines by resident macrophages [53].
Combining several aspects of the studies described above, Lai et al. [55] analyzed curcumin and several analogues for anti-IAV activity. In MDCK cells, treatment with the maximum non-toxic dose of each compound significantly reduced mRNA levels of the IAV M gene in infected cells, with curcumin showing the greatest reduction. Using immunohistochemistry, only curcumin and tetramethylcurcumin inhibited the nuclear export of the IAV nucleoprotein, thus preventing viral assembly. All compounds reduced neuraminidase activity. Consistent with the previous studies, in vivo treatment of mice with 25–100 mg/kg of curcumin reduced lung pathology compared to untreated controls [55]. Additionally, both pre- and post-infection treatment with curcumin improved average survival time of infected mice [55].
Taken together, treatment with curcumin or curcumin analogues can inhibit IAV through several means, including preventing entry [24,55], inhibiting replication [19,55], and preventing exit [24,55]. Additionally, oral treatment with curcumin improved the survival of IAV-infected mice [19,53,55], indicating the potential of curcumin and its analogues against IAV infection.
Though previous research has demonstrated that curcumin can inhibit human enterovirus 71 (EV71) replication in vitro [56], those studies were performed using Vero cells, which are non-human kidney epithelial cells. To better approximate the in vivo conditions of EV71 infection, Huang et al. [20] evaluated curcumin against EV71 in HT29 human intestinal epithelial cells. Treatment with 10 µM of curcumin significantly reduced viral protein expression, genome replication and titer, and prevented EV71-induced cell death. Time-of-addition assays revealed that curcumin did not affect viral attachment and entry, but it effectively inhibited protein expression during early stages of infection [20]. These effects appear to be at least partly due to the ability of curcumin to inhibit protein kinase C-δ (PKCδ). Infection of a cell with EV71 induces phosphorylation of a key activating residue of PKCδ, Tyr311, which is reduced in curcumin-treated cells. Knockdown of PKCδ using siRNA or administration of the PKCδ inhibitor rottlerin also drastically reduced viral protein expression, indicating the importance of PKCδ activation for optimal EV71 gene expression [20]. Treatment with 10–20 µM of curcumin also reduced viral protein expression in C2BBe1 cells that had been differentiated into mature intestinal epithelial cells [20].
For enveloped viruses, direct incubation of curcumin frequently reduces the ability of the virus to infect cells, which is thought to be due to the ability of curcumin to bind to and inhibit the action of surface glycoproteins on the virus [14,15,16]. Somewhat surprisingly, incubation of murine norovirus (MuNoV) with ~679 µM curcumin also significantly lowered plaque formation, despite the fact that noroviruses are non-enveloped [60]. This effect was time- and dose-dependent, suggesting the reduction in plaque formation was due to direct neutralization of viral particles as opposed to preventing infection [60]. However, in human norovirus (HuNoV) replicon-bearing HG23 cells, curcumin had no effect on HuNoV replication [60], suggesting curcumin only affects virus particle integrity and does not alter other aspects of the virus lifecycle.
Li et al. [12] noted while reviewing the genes and pathways impacted by curcumin that there was overlap with pathways controlling the redox reaction of apurinic/apyrimidinic endonuclease 1 (APE1), suggesting curcumin could inhibit APE1 redox reactions. Since Kaposi’s sarcoma-associated herpesvirus (KSHV) replication requires the redox function of APE1 [76], the authors investigated whether curcumin could inhibit KSHV replication. Primary effusive lymphoma (PEL) BCBL-1 cells that were latently infected with KSHV were treated with TPA to induce activation of KSHV and subsequently treated with curcumin. Treatment with 30 µM of curcumin effectively blocked reactivation of KSHV by lowering expression of the switch gene replication and transcription activator (RTA), and the delayed-early gene K8 [12]. Curcumin treatment reduced both the intra- and extracellular KSHV genomic DNA levels (IC50 of 8.76 µM and EC50 of 6.68 µM, respectively) [12], indicating that curcumin is an effective treatment for KSHV infection.
Further curcumin studies specifically in relation to COVID can be found here:
Zinc
Proposed Mechanism: Known to be essential for immune function, and some believe it can inhibit viral replication.
Although antiviral modulation of zinc homeostasis in humans remains unproven, papilloma viruses have evolved mechanisms to alter zinc homeostasis to favor viral replication and persistence (18). The human papilloma virus (HPV) E5 protein can interact with the zinc transporter ZnT-1 in complex with EVER2, thus stimulating nuclear accumulation of zinc (19). The ZnT-1:EVER2 complex responsible for zinc export from the nucleus is inhibited by HPV E5, subsequently increasing both nuclear zinc and the activation of AP1 (20), a transcription factor required for HPV genome expression. Interestingly, homozygous mutations in either EVER1 or EVER2 result in a rare condition termed epidermodysplasia verruciformis (EV). EV patients are particularly susceptible to HPV strains 5 and 8, which significantly increases the risk of developing nonmelanoma skin cancers. HPV strains 5 and 8 lack expression of the E5 protein, which may explain 1) their limited replication in the normal population because of their inability to control zinc homeostasis, and 2) the susceptibility of EV patients to strains 5 and 8 from the loss of EVER protein function, favoring HPV replication. Interestingly, HPV E5 genes have co-evolved with the major HPV oncogenes, E6 and E7, and indicate the potential involvement of E5 in carcinogenesis (21, 22). Clinical trials using both oral and topical zinc have proven effective for the treatment of viral warts, and will be reviewed in a later section.
Metallothioneins, zinc homeostasis, and antiviral activity
Metallothioneins are small, cysteine-rich proteins capable of binding divalent cations such as zinc and copper. As vessels for much of the labile intracellular zinc pool, metallothioneins possess numerous functions through their ability to bind and release metals from their thiol groups. These include storage and transfer of zinc ions and heavy metal detoxification, as well as involvement in oxidative stress, apoptosis, and immune responses (23). Humans express 4 metallothionein isoforms (MT1–4), including the ubiquitously expressed MT1 and MT2 genes (MT1A, B, E, F, G, H, I, J, L, M, X, MT2A), as well as MT3 and MT4 whose expression is limited, and function remains poorly understood (24). Importantly, MT1 and 2 gene expression is extremely responsive to zinc, and therefore serves as an ideal indicator of an individual's zinc status (25). Upon taking a zinc supplement, for example, an increase in protein-bound zinc in the bloodstream is internalized by cells in various tissues and organs through the ZIP transporters. In response to increased intracellular zinc, the metal-responsive transcription factor (MTF1) becomes active, and binds the metal responsive element in metallothionein gene promoters to upregulate their transcription (26). Although there are additional stimuli that influence metallothionein expression, this primarily occurs in a zinc-dependent fashion. Oxidative stress, for example, induces zinc release from metallothioneins as a mechanism to reduce reactive oxygen species generated by mitochondrial dysfunction or viral infection (26). Zinc released from metallothioneins binds MTF1 to stimulate additional metallothionein expression.
It should be noted that metallothioneins, although highly responsive to zinc, have long been classified as interferon stimulated genes (ISGs) (27). IFNs are immunostimulatory cytokines secreted from infected cells and nearby immune cells that induce the expression of hundreds of antiviral genes. They possess diverse roles including chemoattraction, immune cell activation, and direct antiviral activity. In response to IFNs, we suggest that there are 2 mechanisms of metallothionein induction. Most ISGs possess binding sites for STAT- or IFN regulatory factor (IRF) transcription factor-mediated expression, as is the case for MT1X and MT2A (28, 29). Other metallothioneins such as MT1F and MT1G do not possess known IFN regulatory regions in their promoters, but are instead more sensitive to zinc (28). IFNs stimulate an influx of zinc into the target cell, as is the case with some inflammatory cytokines such as IL-6, which in turn drives metallothionein expression.
Because metallothioneins possess such a diverse functional repertoire, their specific roles during viral infection remain undefined. However, both in vitro and in vivo studies have made it abundantly clear that metallothioneins are induced by viruses. The mechanisms often remain undefined; however, metallothionein expression has been attributed to zinc influx or redistribution (19, 28), by viral means, cytokine exposure, or oxidative stress (30). Metallothionein upregulation has been observed in response to measles virus (31), influenza (31, 32), HIV (33), hepatitis C virus (HCV) (34), and coxsackie virus (35), among others. In the case of HIV, zinc appears to be the key driver of metallothionein expression to favor viral persistence. HIV-infected monocytes demonstrate a significant increase in both MT1 gene expression as well as intracellular zinc (33). Elevated intracellular zinc increases monocyte resistance to apoptosis via inhibition of caspase 3 activation [as has been reported previously (36)], thus providing a reservoir for HIV replication. The role of metallothioneins remains unclear in this study; however, they have been described as negative regulators of apoptosis, albeit not through direct caspase 3 inhibition (37). Zinc and metallothioneins also facilitate human cytomegalovirus (HCMV) replication by activating the immediate-early HCMV promoter (38, 39). Kanekiyo et al. demonstrated that both zinc and metallothionein overexpression increased NF-κB binding in the HCMV promoter. Because no complex was detected between metallothionein and NF-κB, it was suggested that metallothioneins served as a zinc donor necessary for NF-κB binding. In addition, as NF-κB transcription factors are known potent activators of HIV and HSV replication, and several other viruses (40), metallothioneins may be proviral. Zinc has also been reported to inhibit NF-κB in numerous studies (41–43). Despite these contrasting data, Kim et al. have bridged these inconsistencies, demonstrating that MT2A can serve as a sink for excess zinc (44), thus limiting its proximity to NF-κB and favoring NF-κB-mediated transcription.
In the case of HCV infection, metallothioneins possess an antiviral role. Using a pan-metallothionein siRNA to knockdown all MT1 and 2 genes, we demonstrated both an increase in HCV replication and a decrease in intracellular zinc content in vitro (34). Interestingly, although ZnSO4 can reduce HCV replication, this effect was ablated when metallothionein genes were knocked down. These data suggest that metallothioneins are either 1) directly antiviral, potentially by sequestering zinc away from viral metalloproteins such as HCV NS5A (45), or 2) indirectly antiviral by acting as zinc chaperones and facilitating antiviral signaling. Further, metallothioneins possess antiviral properties against other viruses as well, as demonstrated in an antiviral screen of 380 human ISGs performed by Schoggins et al. (46). Overexpression of multiple members of the MT1 family inhibited replication of flaviviruses including yellow fever virus and HCV, as well as the alphavirus Venezuelan equine encephalitis virus. This effect was not observed in West Nile virus, and Chikungunya virus. These data indicate that metallothioneins, like many ISGs, are selectively antiviral, perhaps reflecting specific viral zinc requirements during replication. This is particularly evident for HIV, which demonstrated an increase in viral replication as a result of metallothionein overexpression in the Schoggins et al. ISG screen (46), validating previous works (33).
Herpesviridae
The effect of zinc on HSV-1 and -2 has been studied for >40 y, with in vitro studies suggesting that zinc plays an inhibitory role on almost every aspect of the viral life cycle: viral polymerase function (52), protein production and processing (53), and free virus inactivation (48, 54). Although these studies were performed >20 y ago, a more recent study using the zinc ionophore pyrithione demonstrated a reduction in HSV replication from reduced NF-κB activation by interfering with the protein ubiquitination pathway (41). Unfortunately, no recent experimental data can demonstrate with any certainty the mechanism by which zinc inhibits HSV infection. Nonetheless, in vivo studies in mice and humans have shown a significant reduction of infection and disease burden. Mouse studies performing intravaginal zinc inoculation in liquid (55) or gel (56) form both resulted in significant reductions in HSV-2 infection. Several topical zinc application studies have been performed in humans, which demonstrated a significantly reduced recurrence and duration of infection (outbreak) (57–58). The efficacy of topical application, together with in vitro results (48, 54), suggest that free zinc may indeed coat HSV virions, thus preventing infection. Further research into this molecular mechanism is warranted.
Apart from HCMV mentioned above, the effect of zinc on other members of the Herpesviridae family remains unknown because of a lack of clinical data. Mechanistically, zinc ions have been shown to inhibit Varicella-Zoster virus by inactivating free virus in vitro (59). Both HSV and Varicella-Zoster virus belong to the Alphaherpesvirinae subfamily, reflecting their genetic relatedness, and similar mechanism of inhibition.
Picornaviridae
It was clear as early as 1974 that zinc possessed an inhibitory effect on picornovirus polyprotein processing (73). Before 1980, zinc inhibition of picornovirus proteases from human rhinovirus isolates (73, 74), encephalomyocarditis virus (62), poliovirus (61), and foot and mouth disease virus (64, 65) had all been demonstrated. More recent studies using zinc ionophores have illustrated that zinc interferes with the autocatalytic processing of the viral protease 3CDpro into 3Cpro in the picornavirus coxsackievirus B3, thus inhibiting processing of the viral polyprotein (107). However, this was not the case for encephalomyocarditis virus, where zinc appeared to inhibit the tertiary structure within the viral polyprotein (107). Together, these data suggest that zinc may interfere with proteolytic processing of the viral polyprotein because of misfolding, or through direct actions on the viral protease 3CDpro.
Clinical studies using zinc supplementation are primarily limited to rhinovirus infection, and are often grouped with other “common cold” viruses such as influenza and coronaviruses. The majority of studies use zinc lozenges with various zinc formulations and concentrations, possibly explaining the large variability in results [extensively reviewed in (108) and (109)]. Importantly, the amount of ionic zinc present at the site of infection (oral and nasal mucosa) is highly correlated to the study outcome (51, 108), and is dependent on the zinc formulation. At a physiological pH and 37°C, zinc gluconate for example, releases high amounts of ionic zinc, whereas zinc aspartate releases none (108). Upon examining only the relevant studies where high doses of ionic zinc were used, a clear reduction in cold duration of 42% was calculated (109). Whether this was caused by viral inhibition, improved local immune response, or an amelioration of symptoms remains uncertain.
Other respiratory tract infections: influenza, coronavirus, and metapneumovirus
Few studies have examined the antiviral effects of zinc on other respiratory viruses. In vitro replication of influenza (PR/8/34) is significantly inhibited by the addition of the zinc ionophore pyrrolidine dithiocarbamate (110), perhaps through inhibition of the RNA-dependent RNA polymerase (RdRp), as had been suggested 30 y earlier (111). In similar fashion, severe acute respiratory syndrome (SARS) coronavirus RdRp template binding and elongation was inhibited by zinc in Vero-E6 cells (60). Moreover, zinc salts were shown to inhibit respiratory syncytial virus, even while zinc was incubated with HEp-2 cells only before infection, and then removed (72). The authors suggest that this indicates an inhibitory mechanism similar to HSV by preventing viral membrane fusion; however, no measures were taken to assess changes in intracellular zinc content, nor inhibition of other aspects of the viral life cycle.
Flaviviridae: a focus on HCV
Flaviviruses represent a number of insect-borne viruses including dengue and West Nile virus, as well as the hepatotrophic virus, HCV. The effect of zinc on insect-borne flaviviruses is scarce; however, in vitro studies by our group (34) and others (67) have demonstrated that zinc salts can reduce HCV replication (∼50% at 100 µM ZnSO4), perhaps by inhibiting the HCV RdRp, as shown in E. coli [half maximal inhibitory concentration (IC50) ∼60 µM] (66). Although this is a potential mechanism, it has not been examined in eukaryotic cells in which zinc homeostasis is significantly different.
If left untreated, HCV becomes a chronic hepatic infection in around two-thirds of individuals (112), resulting in a significant reduction in plasma zinc (113). Consequently, zinc supplementation in HCV studies have focused on improved patient outcomes, particularly decreased liver inflammation, and enhanced response to antiviral treatment. Supplementation with 150 mg/d polaprezinc (a bioavailable zinc l-carnosine chelate) has been shown to reduce markers of hepatic inflammation alanine aminotransferase and aspartate aminotransferase alone (105), and in combination with the antiviral treatment IFN-α (106). Moreover, polaprezinc significantly improved the rate of viral clearance, particularly in patients with lower viral loads at baseline (102). The mechanisms underlying these observations remain uncertain; however, are likely a combination of direct antiviral effects and strengthening of the antiviral response. Zinc supplementation and the antiviral response is reviewed below.
Togaviridae
Like flaviviruses, togaviruses primarily consist of arthropod-borne viruses such as Semliki Forest virus, Western equine encephalitis virus, and Chikungunya virus. Viral infection occurs by receptor-mediated endocytosis, followed by fusion of virus and endosomal membranes, and particle release into the cytoplasm (114). Using liposome (76), red blood cell (115), and BHK-21 (77) cell model systems, zinc has been shown to efficiently inhibit membrane fusion of Semliki Forest virus and sindbis viruses. Zinc ions interfere with membrane fusion by binding to a specific histidine residue revealed on the viral E1 protein at low endosomal pH (77). Unfortunately, the in vivo relevance of this model is unclear because of the high concentration of zinc (>1 mM) used. Notably, concentrated zinc is present in vesicular zincosomes that are thought to serve as intracellular zinc storage vesicles (116). Similar to the mechanism used by macrophages to inhibit intracellular Mycobacterium spp., zincosome fusion to viral endosomes may inhibit key aspects of the viral life cycle such as togavirus membrane fusion.
Retroviridae: HIV
Retroviruses are named after their ability to transcribe RNA into DNA using their unique reverse transcriptase (RT), consequently allowing integration of retroviral DNA into the host genome. The integrated provirus can then establish a latent infection for the life of the host and is a major barrier to virus cure strategies, particularly for HIV-1 (117). Similar to viral RdRps, zinc has also been identified as an inhibitor of retrovirus RTs (118, 119). Fenstermacher and DeStefano demonstrated in 2011 that Zn2+ cations can displace Mg2+ ions from HIV-1 RT, promoting the formation of an excessively stable, but incredibly slow and inefficient replication complex (70). Zinc was also shown to inhibit the HIV-1 protease in 1991 (68), and to inhibit viral transcription in 1999 (69), but has received little attention since, with the exception of molecular simulation experiments that identified the zinc-binding sites at the catalytic aspartate-25 residue (120). As stated above, HIV can also stimulate zinc influx into monocytes (33), which may appear contradictory based on its antiretroviral properties. Latently infected monocytes and macrophages, however, can act as viral reservoirs for HIV (121), and could therefore benefit from zinc-mediated inhibition of cell death. In fact, unlike the majority of CD4+ T cells, low levels of replication in macrophages do not result in cell death (122), making them a viable reservoir, in addition to long-lived resting CD4+ T cells, for viral recrudescence after cessation of antiretroviral treatment.
Zinc deficiency is common in HIV-infected individuals, where it is associated with inflammation (123), immunological failure (124), and death (125). A recent Cochrane Review examined the role of micronutrient supplementation in people living with HIV (126). Although a number of studies demonstrated beneficial effects of zinc supplementation, the majority were underpowered. The authors concluded that zinc supplementation probably increases blood zinc concentration (moderate certainty), and may increase CD4+ counts (low certainty).
Unlike zinc supplements, prophylactic zinc gels have shown a substantial benefit to limit HIV infection in vivo. Complete protection against vaginal SHIV-RT (a simian HIV virus expressing the human RT) infection in macaques was obtained by pretreating animals with an antiviral gel containing 14 mM zinc acetate and 50 µM MIV-150, a reverse transcriptase inhibitor (127). When used alone, zinc acetate is a potent antiviral, providing 66% protection against SHIV-RT vaginal infection (56) and an EC50 <100 µM in peripheral blood mononuclear cells against a range of HIV strains (128). Importantly, zinc treatment did not affect viral titers in macaques that became infected, nor did it result in zinc resistant HIV mutants with conserved pol (RT) mutations. These data suggest that zinc may not interfere with the HIV RT, but instead inactivate free virus or prevent viral attachment/penetration as reported for HSV (48, 54).
Papillomaviridae
HPVs are oncogenic viruses that infect basal epithelial cells, where they stimulate proliferation resulting in warts. Although cutaneous warts are usually self-limiting and harmless, mucosal strains of HPV (e.g. high risk HPV-16 and -18) are a primary cause of cervical cancers (129). HPV oncoproteins E6 and E7 in particular, are significant drivers of cell proliferation and resistance to cell death by stimulating the degradation of tumor suppressor p53 and pRb, respectively [reviewed in (130)]. Although nuclear zinc appears to enhance HPV replication (see Zinc homeostasis and viral infection), exogenous zinc treatment (CIZAR, zinc chloride and citric acid anhydrous) can effectively inhibit production of viral oncogenic proteins E6 and E7 (71). The inhibition of E6 and E7 by zinc results in apoptosis of cervical carcinoma cells, as they regain the function of tumor suppressors p53 and pRb (71). The mechanism by which zinc downregulates E6 and E7 expression is unknown, but may be preceded by a zinc-driven blockade in another component of the viral life cycle.
Zinc has significant anti-viral properties. Zinc anti-viral effects appear to be virus-specific. Zinc can affect a wide range of viruses. For example, zinc has an inhibitory effect on viral polyprotein cleavage in encephalomyocarditis virus. Zinc inhibits viral RNA polymerase and replication in hepatitis C virus. Zinc can inhibit viral DNA polymerase in herpes simplex virus. In addition, zinc can inhibit reverse transcriptase in HIV. Zinc also has interesting anti-viral effects on respiratory viruses. For example, it can inhibit viral polymerase and polyprotein cleavage in rhinoviruses. The inhibitory effect of zinc on SARS-coronavirus (SARS-CoV) replication has also been reported. Zinc may reduce viral titer in RSV infection [7, 13]. In addition, some zinc-dependent anti-viral proteins, including zinc-finger anti-viral protein (ZAP), play an important role in attenuating viral protein expression in influenza and restricting SARS-COV2 [14, 15]. In this article, we review the most interesting findings regarding the zinc’s role in the anti-viral immune response and immune regulation in the respiratory tract and discuss the importance of this trace element in defense against influenza, RSV, and SARS-COV 2.
Zinc appears to be a key player in anti-viral defense in the respiratory tract. The role of zinc in the immune system can be divided into three categories, namely catalytic, structural, and regulatory functions [27]. Zinc may improve host defense by maintaining the structure and function of the respiratory epithelium barrier. Disorders in the integrity of respiratory epithelium can promote the viruses’ entry [28, 29]. Respiratory tract is constantly exposed to various pathogens; therefore, maintaining the structural integrity of the epithelium is very important in the respiratory system [28]. Zinc depletion in airway epithelial cells disrupted the structural proteins, including β-catenin and E-cadherin, leading to enhanced leakage across the respiratory epithelial barrier [30]. The expression of ZO-1 and Claudin-1 which are tight junction proteins is also found to be zinc-dependent [29]. It seems that zinc deficiency can lead to serious changes in lung epithelial barrier function, possibly through up-regulation of IFNγ and TNFα, enhancement of FasR signaling, and enhancement of apoptosis. In addition, apoptosis and para-cellular leakage can be attenuated by zinc supplementation [30]. One of the most important aspects of anti-viral immune response in the respiratory system is that the immune response must be appropriate and regulated. Although the immune response and the inflammatory process can eliminate pathogens, excessive inflammation can cause tissue damage. Therefore, regulation of inflammation is important, particularly when respiratory cells respond to invading pathogens [31]. It seems that zinc plays a key role in this regard. Inadequate dietary zinc intake can cause Zn deficiency leading to impaired immune function [32]. Zinc is involved in the regulation, normal growth, and function of immune cells such as monocytes, neutrophils, T and B-lymphocytes, dendritic cells, and natural killer (NK) cells. Following a respiratory viral infection, these cells are recruited to the respiratory tissue. It seems that zinc can enhance the proliferation of CD8 + cytotoxic T lymphocytes. These cells are crucial in the immune response to respiratory viruses [33, 34]. Zinc deficiency may impair Th1 cell function; impair the production of IL-1, IL-2, IL-4, and IFN-γ; shift Th1/Th2 balance to Th2; reduce B cell populations; attenuate killing activity of NK cells; and reduce CD8 + T cell population [35–38].
Zinc supplementation may eliminate many of the effects of zinc deficiency on immune cells. It seems that zinc supplementation can increase the numbers of T lymphocytes in older individuals [39]. Moreover, zinc is engaged in the recognition of MHC I by NK cells, and depletion of Zn affects the lytic activity of NK cells [40]. Another study has shown that zinc supplementation in individuals with zinc deficiency leads to an increase in ratios of CD4 + to CD8 + lymphocytes [41]. Besides, zinc is essential for regulation of the balance between the various T cell subdivisions [42, 43]. Experiments in humans demonstrated that decreased zinc content reduces the development of Th1, and thus, the balance between Th1 and Th2 is disturbed. Th1/Th2 imbalance is eliminated via zinc supplementation [44]. Zinc deficiency reduces the production of antibodies and the number of B lymphocytes [34]. Zinc may reduce excessive inflammatory response by modulating Treg functions [45]. In Treg development, two zinc-dependent molecules of IRF-1 and TGF-β-induced Smad 2/3 signaling are involved [46]. Zinc supplementation enhanced TGF-β-induced Smad 2/3 signaling and dampened IRF-1 activity [47]. Zinc deficiency resulted in increased NF-κB expression in the lungs, leading to up-regulation of target genes, including ICAM-1, TNFα, and IL-1β [48]. In addition, it seems that zinc deficiency can lead to enhanced production of pro-inflammatory cytokine (TNFα, IL-6, CXC L1), enhanced migration of neutrophils, and increased production of CXC L1 and IL-23 by macrophages, possibly through NF-κB activation [49]. By inhibiting dephosphorylating enzymes, such as protein tyrosine phosphatases (PTP), zinc can directly regulate immune system activity [50]. PTPs can regulate TCR signaling [51]. It seems that inhibiting PTP1B expression may increase the expression of CXCL1, CXCL9, and CXCL10 during RSV infection [52]. Therefore, PTPs may be important during respiratory viral infection. As mentioned in the previous section, interferons (IFNs) are inflammatory stimulus and play a key role in orchestrating adaptive and innate immunity system [52]. In vitro zinc therapy has been shown to increase the production of IFNα by white blood cells [53]. It is proposed that zinc may stimulate the up-regulation of anti-viral enzymes including protein kinase RNA-activated (PKR) and latent ribonuclease (RNase L). These enzymes are important in type I IFN anti-viral activity [5, 54]. It seems that high doses of zinc can inhibit IFN-γ production and lymphocyte function [44]. Therefore, zinc may also have immunosuppressive effects.
The relationship between Zinc and IFN-λ is also interesting. One study showed that zinc with interfering in IFN-λ 3 binding to IFNL receptor 1 can act as a specific and potent inhibitor of IFN-λ 3 signaling. Strong zinc-mediated inhibition of IFN-λ3-induced CXCL10 expression has also been demonstrated in vitro, indicating the biological complexity of zinc [55]. In addition to these, the intracellular availability of zinc may play an important role in anti-viral activity [56]. Zn transport is principally mediated by two major transporters: (1) the zinc transporter (ZnT) or solute carrier 30 (SLC30) family and (2) the zinc importer (ZIP), Zrt (zinc-regulated transporter)-like, Irt (iron-regulated transporter)-like proteins, or solute carrier 39A (SLC39A) family [57]. Currently 10 members of the ZnT (ZnT 1–10( family and 14 members of the Zip family (ZIP 1–14) have been identified [58]. ZnT transporters reduce intracellular Zn2+ by efflux of Zn2 + from the cytoplasm to outside the cell or influx into cellular organelles, such as lysosome and endoplasmic reticulum (ER). ZIP transporters, which carry out the opposite role, increase intracellular Zn2+ by influx and import of Zn2+ into the cytoplasm from outside the cell or cellular organelles [59]. It seems that zinc transporter SLC39A8 (Zip8) is abundantly expressed in the lung [60]. In lung epithelial cells among the ZnT and ZIP transporter genes, only ZIP8 is strongly induced by TNF-α. Thus, Zip8 is a critical regulator in zinc-mediated cyto-protection and plays a role in the survival of lung epithelial cells [61]. Besides, Zip8 controls IFN expression by regulating zinc release from lysosomes [62]. It seems that Zip8 expression in human monocytes can also be up-regulated in response to LPS [63]. There seems to be an interesting relationship between the NF-kB signaling pathway, and zinc transporters, especially ZIP8. It seems that NF-kB activity may be regulated by zinc during innate immune response [48]. Studies have shown that zinc plays an important role in regulating the activity of the NF-kB signaling pathway, and this regulation may be cell-specific [64, 65]. It seems that zinc can induce anti-viral response and inhibit dengue virus replication in lung epithelial cells and control viral infection by activation of NF-KB signaling pathway [66]. Besides, ZIP8 is a potent negative feedback regulator of NF-kB. ZIP8 can negatively regulate immune balance by directing zinc into the cytosol, leading to inhibition of IkB kinase (IKKb) [63]. An in vivo study showed that zinc supplementation induced the expression of Zip8 and ameliorated lung injury [67].
IL-23 and CXCL1 production and airway neutrophil infiltration are increased in ZIP8-deficient mice following bacterial infection [68]. ZnT1, ZnT4, and Zip1 transporters are expressed in the lung tissue. ZIP1 and ZIP2 are also present in lung alveolar macrophages and appear to play an important role in the efferocytosis activity of these macrophages [69, 70]. Paracrine or autocrine signaling in response to type I IFNs (IFN-α/β) can lead to up-regulation of a wide array of IFN-stimulated gene (ISG) products which can target viruses life cycle [71]. One of the ISG products is zinc-finger anti-viral protein (ZAP) encoded by the zinc-finger CCCH-type, anti-viral 1 (ZC3HAV1) gene. ZAP is a member of the poly (ADP-ribose) polymerase (PARP) family [71, 72]. One study showed that ZAP and its cofactors TRIM25 and KHNYN are expressed in lung cells. It seems that ZAP can bind to CpG dinucleotides regions of viral RNA in lung cells [15]. ZAP does not have enzymatic activity and exert preventive effects against viral replication through interaction with TRIM25 and KHNYN [73]. A20 protein is another important zinc-finger protein. This protein is also known as TNFα-induced protein 3 (TNFAIP3). A20 is a cytoplasmic protein that is composed of two domains: a C-terminus domain built up by a unique seven zinc-finger structure with ubiquitin-binding activity and an N-terminus ovarian tumor (OTU) domain with deubiquitinase activity [74]. The A20 protein is a negative regulator of TLR, retinoic acid-inducible gene 1 (RIG-I)-mediated signaling, IRF signaling pathway, and NF-KB signaling pathway [75–77]. A20 can effectively regulate NF-kB signaling via affecting a range of related factors including,TNF receptor-associated factor 6 (TRAF6: TRAF pathways), NF-KB essential modulator (NEMO), receptor-interacting protein 1(RIPl), tumor necrosis factor receptor 1 (TNFR1), CD40, toll-like receptors (TLRs), NOD-like receptors (NLRs), and the interleukin-1 receptor (IL-1R) [40, 78]. It seems that inhibition of A20 expression in respiratory epithelium can enhance the protection against influenza infection. In later stages of infection, this improved protection may be associated with suppression of CCL2 expression and modulation of pulmonary cytotoxic T cell [79]. A study on RSV-infected cells showed that down-regulation of A20 can increase apoptosis and induce an innate immune response in infected epithelial cells [80]. Zinc exerts an inhibitory effect on the activation of NF-kB by inducing the A20. It seems that A20 can inhibit NF-kB, possibly through inactivation of TRAF6 [81, 82].Therefore, it seems that zinc can decrease the production of pro-inflammatory cytokines such as IL-1β, and TNF-α via up-regulation of A20 leading to attenuation of NF-kB [32]. It has been suggested that zinc supplements may affect NF-kB activity by altering A20 activity [83].
The zinc-dependent metallopeptidase STE24 (ZMPSTE24) is another zinc-dependent protein that can act as a broad-spectrum anti-viral protein. This protein is an essential inhibitor of viral entry and can restrict wide range of viruses including influenza and Ebola [50, 84]. Increased viral load was reported in the lungs of ZMP STE24-deficient mice following influenza infection [85]. ZMPSTE24 expression is necessary for interferon-induced transmembrane protein (IFITM) activity. This protein can prevent viral entry [84, 85]. Autophagy likely acts as both an anti-viral and pro-viral pathway in the pathogenesis and life cycles of a wide range of viruses [86]. Increasing evidence indicates the idea that in the autophagy process zinc may be a positive regulator [87–89].
The influenza virus is a known main factor of acute respiratory disease, which is extremely contagious and transmitted from person to person via respiratory droplets. Airway epithelial cells are the main target of the virus for attack and replication. Influenza virus can cause seasonal respiratory infection and associated pandemic [90, 91]. The flu pandemic has occurred many times. The H2N2 (1957), the H3N2 (1967), the H1N1 (2009), and the H1N1 (1918) pandemics are among the most important of flu pandemics. The pandemic of the influenza virus, which happened in 1918, was terrible, and 40–50 million peoples have been died [92]. Based on various nuclear proteins (NP) and matrix proteins (M), there are four groups of influenza viruses (A, B, C, D). A and B types of influenza virus are the main causes of influenza infection in humans [93]. Influenza viruses belong to the Orthomyxoviridae family. The virus consists of one chain negative-sense RNA genome that includes eight-segmented in A and B type [94, 95]. Binding each of the vRNA fragments to heterotrimeric polymerase complex is required for ribonucleoproteins (RNP) formation [96]. Because the influenza virus replicates in the host cell nucleus, RNP must be transported to the nucleus. In this process, there is interaction between the RNP and cellular transport systems [97].Hemagglutinin (HA) and neuraminidase (NA) are important glycoproteins. These proteins are presented on the external surface of the virus [98]. Influenza viruses are divided into different subtypes based on HA and neuraminidase NA [99]. H1N1 and H3N2 are among the most important of these subtypes in influenza A and are considered as the main causes of seasonal influenza [100].
HA has a key role in virus entry into the host cell and primary phase infection. When the globular head of HA adjoins to the sialic acid receptor in the respiratory tract epithelial cell, the replication cycle of the influenza virus can start [101, 102]. After this step, clathrin-mediated endocytosis has occurred, and then, the endosome is formed [103]. The combination of virus and endosome membrane is facilitated by acidic conditions in the late endosome, which leads to structural change in HA and starts a progression of events that can cause viral ribonucleoprotein (vRNP) releasing into the cytoplasm. Finally, vRNA goes into the nucleus [96, 104–106]. After entering the viral ribonucleoprotein into the nucleus, RNA-dependent RNA polymerase, which is part of vRNP, uses negative-sense viral RNA as a template to make two types of positive-sense RNAs [95, 105]. One of these RNAs is viral mRNAs, which encode viral proteins, and the other is complementary RNA, which is transcribed into negative-sense viral RNA. Negative-sense viral RNAs are assembled with viral proteins and form viral particles. Viral particles are released through budding. HA and NA play a key role in viral particle releasing [95, 107, 108]. The primary anti-viral reaction against influenza can lead to the secretion of and type I IFNs and pro-inflammatory cytokines such as TNF-α and IL-6 [109, 110]. Immune cells are recruited to the site of infection to control the spread of the virus. Excessive and uncontrolled production of a pro-inflammatory cytokine called “cytokine storm” can cause tissue damage and organ failure [111, 112]. Due to mutations that may occur during replication in the virus genome, mutant virus can be produced, leading to the virus becoming resistant to existing antibodies and escape from neutralization [113, 114]. Therefore, recognizing alternative anti-influenza factors with various mechanisms is of importance. Due to zinc’s role in anti-viral defense and immune regulation, several studies have investigated the importance of zinc in influenza infection. The findings of an interesting study showed that zinc oxide nanoparticles have an anti-viral effect only after a viral infection of the cells, which finally leads to a decrease in viral titer [115]. Zinc appears to be able to inhibit influenza virus’ RNA polymerase activity [116]. A recent study showed that zinc-finger protein ZFP36L1 has anti-viral properties and can enhance host anti-viral defense against influenza A virus by attenuating the production of viral proteins including HA, M, and NS [117]. In the previous section, we discussed the importance of zinc-finger anti-viral protein (ZAP). One study showed that the short isoform of this protein (ZAPS) could inhibit the expression of influenza viral proteins including PA, PB2, and NA [14].
SOD1 is a crucial zinc-dependent antioxidant enzyme. It appears that this enzyme can significantly attenuate viral polymerase activity and has anti-viral properties against H1N1IAV infection. It seems that repression of the copper-zinc SOD1 enzyme by the IAV may facilitate virus replication by disrupting cell redox balance [118]. As mentioned in the previous section, ZMPSTE24 is also an important zinc-dependent protein involved in anti-viral defense and immune regulation. One study showed that IAV-infected ZMPSTE24-deficient mice had increased viral burden, cytokine production, and mortality, indicating an important role for this zinc-dependent protein in anti-viral defense, and immune regulation following IAV infection [85]. Zinc-finger CCCH-type anti-viral protein 1 (ZC3HAV1) is another zinc-dependent protein involved in the anti-viral defense of host cells. One study showed that this protein could attenuate IAV replication by increasing IFN-β expression [119].
Although very few studies have been conducted on the importance of zinc and zinc-containing proteins in RSV infection, the findings indicate that zinc is helpful in controlling RSV infection. It seems that blood zinc level in children with RSV pneumonia is significantly low [5, 137]. In one exam, the inhibitory effects of zinc on RSV infection were seen, when incubated with human epithelial type 2 (HEp-2) cells only before infection [138]. Studies also have shown that zinc treatment enhances interferon α (IFNα) production by leukocytes. IFNα, an immune-stimulatory cytokine, has anti-viral activity. Increasing the expression of anti-viral genes by IFNα that are correlated with degradation of viral RNA as well as inhibition of viral RNA translation is proposed to be stimulated by zinc [5, 7]. The studies also reported that intake of at least 75 mg zinc per day could decrease the duration of pneumonia symptoms [139]. Therefore, it is necessary to study the relationship between zinc supplementation and RSV-induced pneumonia. One study showed that fetal ethanol exposure could be associated with immunosuppression and reduced RSV phagocytosis. However, maternal zinc supplements could enhance RSV phagocytosis and reduce RSV burden in the lungs [140], indicating the importance of sufficient zinc levels in the neonatal immune system. Undoubtedly, further studies could reveal more dimensions of the benefits of zinc in controlling RSV infection. Studying the role of zinc-dependent anti-viral proteins in RSV infection can be very helpful and should be considered in future studies.
It seems that zinc can attenuate the RNA synthesis of SARS-COV and have an inhibitory effect on replicating this virus [13]. Besides, one study showed that zinc could inhibit papain-like protease 2 (PLP2) of SAPS-COV [147]. This enzyme is very important in virus virulence. Since there are many similarities between the SARS-COV and SARS-COV2 genomes, it is necessary to study the above-mentioned results inSARS-COV2 infection carefully. Clinical studies in patients with COVID-19 have also reported interesting results. One study showed that serum zinc levels in patients with COVID-19 were significantly lower than in the healthy control group. In addition, the findings of this study showed that ARDS rate, length of hospital stay, and mortality increased in COVID-19 patients with zinc deficiency [148]. A study of pregnant women with COVID-19 showed that serum zinc levels in these patients were significantly reduced compared to the control group. Besides, an inverse correlation was reported between serum zinc and IL6 levels. There also appears to be an inverse correlation between zinc/copper ratio and disease severity in pregnant women with COVID-19 [149]. Another study showed that normal levels of zinc and selenoprotein P were associated with higher survival in patients with COVID-19 [150]. The results of some studies have shown that zinc can be effective in the treatment of COVID-19 and increase the effectiveness of drugs such as hydroxychloroquine and azithromycin. One study of 3473 patients with COVID-19 showed that a combination of zinc and ionophore hydroxychloroquine could reduce the in-hospital mortality rate by 24%; in contrast, zinc alone or ionophore alone could not reduce mortality [151]. One study showed that zinc sulfate, along with hydroxychloroquine and azithromycin, could reduce ICU admission, need for ventilation, and mortality in hospitalized patients with COVID-19 [152]. Another study of outpatients with COVID-19 showed that treatment of these patients with low-dose hydroxychloroquine and azithromycin combined with zinc could reduce hospitalization rates and mortality rates [153].
Further studies can be found here:
And here:
And here:
Selenium
Proposed Mechanism: An antioxidant that is thought to boost the immune system, potentially helping the body clear latent viruses.
Selenium (Se), an essential trace element in humans, has a long history of lowering the occurrence and severity of viral infections [5,6,7,8,9]. Se deficiency impacts immune function [10], viral expression [8], selenoprotein expression [11], and alters antioxidant response [12], allowing for greater susceptibility to severe viral and bacterial infections [13]. Supplementing the diet with Se has demonstrated positive effects on enhancing immunity against viral attacks [5]. Much of the benefits derived from Se are due to its incorporation into selenocysteine, an important component of the antioxidant defense systems, including the regulation of glutathione peroxidase (GPXs) and thioredoxin reductase (TXNRD) activities [14]. Low levels of Se can lead to more severe forms of viral infections and adequate selenium levels may provide a protective effect toward the host response by affecting both immune response and oxidative stress [13,15]. Severe pathology in Se deficiency is evidenced by more frequent and graver symptoms, higher viral loads, declining levels of antioxidant enzymes such as GPX, and mutations to the viral genome. Studies conducted by Beck et al. described in this review, demonstrate that Se-deficiency is capable of increasing the virulence of a benign coxsackie virus through viral mutations and these mutations have led to a reduction in GPX activity, therefore, resulting in oxidative stress [13,15].
4.1. Coxsackie Virus
Several decades of research have provided sufficient evidence to demonstrate a relationship between Se deficiency and Keshan disease, a grave cardiomyopathy. This cardiomyopathy is believed to be caused by infection with Coxsackie B virus, a nonenveloped single-stranded RNA virus pertaining to the Picornaviridae family, and exclusively found within China [10,45]. It was later discovered in the 1970s and 1980s that much of the Se levels in the soil, water, food, and human circulating fluids in areas affected by Keshan disease were deficient compared to other neighboring Chinese providences [46]. Sodium selenite was provided to the population and a prospective study showed that it prevented Keshan disease. Keshan disease was eradicated from endemic areas after the government enacted a Se supplementation policy, therefore, demonstrating that Keshan disease occurred due to two factors, infection with Coxsackie B virus and Se deficiency [47,48,49].
Animal studies conducted by Beck et al. confirmed the relationship with Se in mice by infection with a non-cardio-virulent strain of Coxsackie B virus (CVB3/0) and a myocarditic strain (CVB3/20). Heart damage was only observed in the mice fed a Se-deficient diet compared to mice fed a Se-sufficient diet for 4 weeks, and the typical human pathology was also observed [28,50]. These studies illustrated that Se deficiency caused a virus that was non-virulent to contribute towards the development of myocarditis in the host, and also increased its pathogenicity as the cardiovirulent strain under Se deficiency produced greater symptoms [28,51].
Additional observations by Beck and colleagues showed higher viral loads in the Se-deficient mice infected with both CVB3/0 and CVB3/20. The Se-deficient mice were found to have reduced T-cell expansion and diminished mRNA levels of cytokines compared to Se-adequate mice [15]. Subsequent studies led to the finding that Se deficiency was responsible for a change in the genotype of the benign coxsackie virus CVB3/0 that caused it to become virulent. Specifically, six nucleotides were modified that mimicked other virulent strains of CVB3 viruses. Due to these mutations, the virus now had the possibility to become pathogenic even in a Se-adequate host [45]. It was then hypothesized that a reduction in GPX activity was responsible for the viral mutations. Therefore, subsequent studies were conducted to demonstrate the protective effect of GPX1 in developing heart damage when infected with a benign strain of Coxsackie B virus (CVB3/0) [52]. Mice with a disrupted gpx1 gene infected with CVB3/0 compared with wild type mice with an intact gpx1 gene experienced myocarditis, and sequencing of the viruses from the mice with disrupted gpx1 gene showed seven nucleotide changes in the Coxsackie virus. Interestingly, six of the seven nucleotide changes in the genome of the virus from the mice with disrupted gpx1 genes matched the changes found in the Se-deficient mice previously [52]. These classic experiments exhibit how nutritional status as it pertains to Se, and its ability to protect antioxidant systems and immunity may impact the potential evolution of viruses to become more virulent.
4.2. Influenza
Influenza viruses, known to cause the flu, are enveloped, single-stranded RNA viruses within the Orthomyxoviridae family. Selenium deficiency has been associated with poor selenoprotein expression [11] and altered antioxidant response in viral influenza A infection [12]. The elegant in vitro [13] and animal experiments conducted by Dr. Beck et al. [28,45,46,50,52,53] were the first to demonstrate the detrimental effects of Se deficiency in influenza A virulence, which occurred due to changes in the viral genome [54]. Se deficiency in mice infected with a highly virulent Influenza A strain (Influenza A/PR/8/34), however, had higher levels of IL-2 expression followed by a higher level of IL-4 expression in the lung, and higher survival compared to Se-adequate mice. These studies demonstrated the essential role of Se in mounting an immune response to influenza A, by changing its virulence and altering the host’s immune response [55].
These in vitro and animal studies suggested that in vivo Se supplementation might have a beneficial effect in humans, especially in the elderly, as the immune response is compromised by age. To test this hypothesis, Ivory et al. [56] conducted a 12-week randomized, double-blinded, placebo-controlled clinical trial in six groups of individuals with suboptimal Se status or plasma Se levels < 110 ng/mL to observe the response after the flu vaccine was provided. Four groups were given daily capsules of yeast: 20 participants were given 0 μg Se/day (placebo), 18 participants were given 50 μg Se/day, 21 participants received 100 μg Se/day, and 23 received 200 μg Se/day. Two groups were given onion-containing meals, 17 participants received < 1 μg Se/day (unenriched onions), and 18 participants received 50 μg Se/day (Se enriched onions). After 10 weeks of supplementation, all participants were administered the flu vaccine. Selenium supplementation compared to placebo had beneficial and detrimental effects on the cell immunity response to the flu vaccine that was dependent on the type of Se, and dose administered [56]. Se-yeast dose of 200 µg/day demonstrated enhanced IL-10 secretion and lower granzyme B content, a cytotoxic protease that induces apoptosis of target cells, within a cluster of differentiation 8 (CD8) cells, while 50 µg/day of Se through the enriched onion meal increased granzyme content and perforin in CD8 cells and reduced natural killer T-cells.
The effectiveness of antiviral agents such as amantadine (AM) [57], oseltamivir (OTV) [58], β-thujaplicin (TP) [59], and ribavirin (RBV) [60] to combat viral influence has been limited by the emergence of drug-resistant viruses. Biological Se nanoparticles are increasingly used as an agent to diminish drug resistance by “decorating” the nanoparticles with antiviral drugs to increase effectiveness, such as Se@AM, Se@OTV, Se@TP, Se@RBV. Selenium nanoparticles have been found to decrease oxidative stress, induce apoptosis of infected cells, and reduce lung cell damage during influenza infection, in addition to having low toxicity and increased drug activity in murine [59] and in vitro models [60].
4.3. Human Immunodeficiency Virus (HIV)
It is estimated that over 37 million people globally are living with HIV [61]. HIV is an enveloped, single-stranded RNA virus and without treatment causes a collapse of the immune system. The prevalence of Se deficiency in people living with HIV (PLWH) is reported to be around 7–66% and increases as HIV disease progresses over time [62,63,64,65]. Although antiretroviral therapy (ART) has allowed HIV disease to become a chronic disease, the immune system is still not fully reconditioned [66]. The rate of Se deficiency in PLWH in Sub-Saharan Africa is greater than that in the United States (U.S.A.) and the literature shows lower Se soil content in Sub-Saharan Africa [67]. Selenium deficiency in HIV disease is associated with disease progression and mortality, regardless of ART initiation [63,68,69,70,71]. Models of simian immunodeficiency virus also corroborate the relationship between Se deficiency and disease progression [72].
The relationship between HIV disease and increased oxidative stress [73,74,75,76,77,78] was recorded early in the disease, and the development of ROS and its association with HIV disease progression was documented in the very early stages of the emergence of the disease [79,80]. Lower GSH levels were found as HIV advances to acquired immunodeficiency syndrome (AIDS) [81] and alterations in antioxidant defense systems (SOD, CAT, and GPX) have also been observed in PLWH [75,77,82]. Supplementation of 250 µg of L-selenomethionine (100 µg of Se) for one year led to increased GPX activity [83] and adequate dietary Se intake was also associated with lower oxidative stress in PLWH [84].
Studies in children and adults living with HIV have found associations with Se deficiency and adverse health outcomes including mortality. Countries with a high prevalence of HIV such as South Africa, have shown that Se intake in children is not adequate and the overall diet quality is low [85]. In studies conducted in Nigeria, children with HIV had significantly lower Se levels compared to matched HIV-non-infected children in the same region and a high rate (>70%) of Se deficiency [86,87]. In children living with HIV in the U.S.A., Se deficiency was associated with advanced immunodeficiency [88] and mortality [63]. In adult PLWH who were initiating antiretroviral therapy (ART) or were already taking ART, Se deficiency was associated with HIV disease progression and mortality [70,71]. Additionally, Se values have been found to be lower in adult PLWH than in adults without HIV [89,90], as well as in later stages of HIV [90].
Several Se supplementation trials have been conducted within the United States [91,92], Tanzania [93,94], Botswana [95], and Rwanda [96]. These trials have demonstrated that Se supplementation in the dose of 200 µg in PLWH who are ART naïve or on ART may delay HIV disease progression through maintenance of cluster of differentiation 4 (CD4) cell counts. Hurwitz et al. [92] demonstrated that supplementation with Se resulted in significantly suppressed HIV viral load along with improved CD4 cell count. Trials using Se as part of a formula in combination with other micronutrients have not been able to discern the benefits of Se from the other components. We [95] concluded that supplementation with multivitamins and Se was safe and statistically significantly reduced the risk of immune decline and morbidity. Discrepancies between supplementation studies include the ART status of the participants, the baseline CD4 cell counts, and the length of time that the participants were supplemented and followed [97]. A Cochrane review of micronutrient supplementation and HIV concluded that additional trials with single nutrients were needed to build the evidence base for adults and establish long-term benefits [98].
4.4. Hepatitis B and C Viruses (HBV and HCV)
The World Health Organization (WHO) estimates that 257 million people and 71 million people were infected with hepatitis B virus (HBV) and hepatitis C virus (HCV), respectively [99]. Both HBV and HCV can cause acute and chronic hepatitis which can develop into cirrhosis and hepatocellular carcinoma (HCC). In 2015, there were 720,000 and 470,000 deaths from hepatic cirrhosis and HCC, respectively [99]. Though both HBV and HCV are hepatotropic, HCV belongs to the Flaviviridae family, whereas HBV is a member of the Hepadnaviridae family [100]. HBV is a partially double-stranded DNA virus that uses the host RNA polymerase II machinery to produce pre-genomic RNA, which is reverse transcribed into viral DNA [101]. HCV is an enveloped, single-stranded RNA virus, which exhibits extremely high mutation rates—up to one mutation per genome per generation cycle—since proofreading activity is lacking in RNA-dependent RNA polymerases required for its replication [102].
Selenium status determined by GPX3 activity and the concentration of serum/plasma Se and plasma SELENOP have been reported to be influenced in HBV and HCV patients in several studies. Serum Se concentrations are statistically significantly lower in HBV/HCV infected people when compared with the control group [103,104]. Selenium level is also associated with the severity and progression of the HBV/HCV disease [103,105,106]. Increased concentrations of aspartate aminotransferase and alanine aminotransferase (ALT) were independently associated with low Se concentration in chronic HBV patients with more hepatic damage [106]. The Se concentrations in plasma and erythrocytes are significantly lower in HCV-infected people than in controls and have an inversed correlation with HCV viral load [107]. Besides this, plasma Se level is statistically lower in people with HCV-induced cirrhosis with and without HCC when compared with HCV-infected people without liver cirrhosis or HCC [108].
Chronic HBV and HCV infection enhances ROS production and cause elevated oxidative stress and decreased antioxidant activity in liver cells [109,110,111,112]. ROS, produced as byproducts during cellular metabolism, have been implicated in several hepatic pathologies to maintain cellular homeostasis, including cell signaling, transcription, apoptosis, and immunomodulation [113,114,115,116]. Patients suffering from HBV or HCV infection show significant depletion of GSH and GPX when compared to non-infected participants [117,118]. As part of the antioxidant defense system, Se deficiency may be enhanced by the hepatic viral-induced oxidative stress and the requirement of selenoproteins during viral replication. An in vitro study showed that HCV can inhibit the expression of gastrointestinal-GPX (GPX2), a GPX that is also expressed in the liver, resulting in an increase in viral replication [7,119]. Nonstructural protein 5A (NS5A) of HCV, which is reported to enhance oxidative stress by perturbing Ca2+ homeostasis [120], also induces the expression and activity of GPX1 and GPX4 [121]. Besides, the GPX homology region overlaps the highly conserved NS4 gene in HCV, supporting that the NS4 gene is a functional GPX module [122]. Although the causes of Se deficiency in HBV and HCV are not fully understood, it is possible that the decreased level of circulating Se is related to the requirement of Se during viral replication.
The demand for Se during HBV and HCV infection causes the systemic deficiency of Se and can be compensated by supplementation. Supplementation of Se has shown to be protective against a wide range of different sources of oxidative stress and optimal immune responses [123,124]. Primary HCC incidence was reduced by 35.1% in Se supplemented people living with HBV as compared with non-supplemented people living with HBV [125]. However, when Se supplementation was stopped, primary HCC incidence began to increase [125]. Selenium also improves the rate and level of antibody response against the HBV vaccine in insulin-dependent diabetes mellitus cases that were on an accelerated vaccination schedule instead of a routine vaccine schedule [126]. A triple antioxidant combination of Se, alpha-lipoic acid, and silymarin supplementation in three chronic HCV-infected patients demonstrated an improvement in ALT [127]. However, a 6-month trial showed that those living with HCV supplemented with vitamins C, vitamin E, and 200 μg Se per day had an increase in antioxidant status with no beneficial effect on ALT, HCV viral load, or liver damage as compared with the non-supplemented individuals living with HCV [128].
As discussed in the previous paragraph, Se deficiency has been involved in the pathogenesis of HBV and HCV infection. In turn, the deficiency of Se leads to elevated oxidative stress, pathological changes, and inflammation in the liver [129]. Histological study shows hepatic sinus expansion, lymphocyte infiltration, and stripe-like hyperplasia in the liver with Se deficiency. Liver inflammation is initiated by Se deficiency as pro-inflammatory factors and molecules, such as IL-1β, IL-6, IL-12, NF-κβ, and NF-κβ p65, were all significantly higher in the Se-deficient group [129]. Hepatic antioxidant capacity is also influenced by Se deficiency as a decrease in both mRNA expression of selenoprotein genes (GPX1 and GPX3), as determined by quantitative real-time PCR and the level of selenoproteins (GPX1, GPX4, and TXNRD1), identified by global proteomics, are observed [129,130,131]. Interestingly, an in vitro study showed that Se deficiency can result in oxidative stress and apoptosis of non-HBV-infected hepatocytes, whereas HBV-infected hepatocytes gain a survival capacity and escape from the apoptosis consequence [132].
4.5. Poliovirus
Poliovirus is part of the Picornaviridae family of RNA viruses that are non-enveloped and may infect vertebrate animals [133]. Infection generates high levels of ROS and reactive nitrogen species as well as antioxidant enzymes being downregulated within cells that have been infected [134]. The supplementation of Se has been shown to improve the response of the vaccine for the poliovirus more in patients that have less optimal immune systems based on Se status, although the impact of supplementation on patients with optimal immune systems based on Se status is unclear [135]. Furthermore, the supplementation of Se did not affect all aspects of an individual’s immune response shown in the same trial where a live poliomyelitis vaccine was given to people with low Se status. This resulted in the increase of T cell and IL-10 production but did not affect the natural killer (NK) or B cell count, still resulting in the rapid removal of poliomyelitis from the patients supplemented [136]. Selenium also did not affect the levels of CD4+ T helper (Th) 1 cells to Th2 cells or the humoral immune response [135] in a different trial where patients were given a dose of the poliovirus vaccine and took either a placebo, 50 µg or 100 µg of Se. An increase in the antibody titers within all groups that were relatively equal was shown [135]. Se supplementation prior to the polio vaccine seemed to only enhance the cellular antiviral immune response.
4.6. Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2)
The novel COVID-19 is caused by SARS-CoV-2, a single-stranded RNA coronavirus. The severity of the disease has been linked to aging and comorbidities such as hypertension, diabetes, obesity, cardiovascular disease, kidney disease, cancer, and pulmonary diseases [137,138]. Most of the people who test positive for COVID-19 develop mild or no symptoms, while others develop acute respiratory distress syndrome (ARDS), heart failure, blood clots, neurological complications, and elevated inflammatory response [137,139]. SARS-CoV-2 pathology has been associated with an increased immune response, leading to a release of cytokines and chemokines, also known as cytokine storm [140], as well as increased inflammatory markers such as D-dimer and ferritin [141,142]. This hyperactive inflammatory response may also bring about severe pathology in the brain [143]. SARS-CoV-2 may directly impact the central nervous system and enter the brain through various routes [144,145,146,147]. Increased systemic inflammation promoted by SARS-CoV-2 has the potential to disturb the blood-brain barrier and co-morbidities associated with severe cases of COVID-19 may enable the attack of the brain by SARS-CoV-2 [143,148].
It has been noted that there is a potential and developing relationship between Se levels and COVID-19 outcomes. Proposed mechanisms by which Se may act upon the SARS-CoV-2 virus based on previous research in RNA viruses include restoration of GPX and TXNRD thus reducing oxidative stress, reduction of viral-induced cell apoptosis, provision of Se for the host’s antioxidant needs, protection of endothelial cells, and reduced blood platelet aggregation [149,150]. COVID-19 is associated with a heightened level of oxidative stress and inflammation that are implicated in the pathogenesis of pulmonary disease [151]. GSH provides protection to the epithelial barrier within the lungs, and it has been suggested that improvement of GSH levels would be a strategy that may protect against inflammation and oxidant-related damage in the lungs [151]. A study conducted by Mahmoodpoor et al. [152] supplemented sodium selenite in patients with ARDS, often associated with severe cases of COVID-19, and found that it restored the antioxidant capability of the lungs, reduced inflammation, and improved respiratory mechanics. Lower total lymphocytes and CD4+ T, CD8+ T, B, and NK cells were found in COVID-19 patients and those with severe cases compared to mild cases of COVID-19 had lower lymphocyte subsets [153]. The function and differentiation of B and T cells may be affected by Se status [154]. Deficiency of Se in mice has been associated with lower T cell proliferation, while supplementation increased T cell activity and differentiation [155].
Clinical data investigating Se and COVID-19 are sparse; however, some reports from China and other countries globally have surfaced. In China, where there is a wide range of soil Se levels and thus a variation of Se daily intake, a linear association has been demonstrated between reported cure rates of COVID-19 and Se hair concentration data, dating from 2011 and older [156]. The same research group in China documented higher fatality risk in cities that had selenium-deficient levels in crops and topsoil compared to cities with non-deficient selenium levels in crops and topsoil [157]. Intake of Se varies worldwide, and China is known to be one of the most Se deficient countries in the world, with a wide range of levels that differs from lowest to highest in the world. COVID-19 fatality rate varies across different regions in China, suggesting that Se status may be related to COVID-19 outcomes [156,158]. In the city of Wuhan, where the SARS-CoV-2 virus was first discovered, and in other cities such as Suizhou and Xiaogan, low Se soil status was associated with the highest COVID-19 incidence [156]. In contrast, cities such as Enshi, Yichang, and Xiangyan, where high Se intake occurs, had the lowest COVID-19 incidence [156]. In contrast, in a retrospective study completed in Wuhan, China, with hospitalized COVID-19 patients, the severity of COVID-19 was associated with higher Se levels in urine [159]. The authors hypothesize that liver abnormalities due to the severity of the disease may have impacted the excess urinary Se found in severe COVID-19 patients [159].
Studies conducted in other parts of the world are showing similar relationships to those completed in China. In a study conducted in South Korea on hospitalized COVID-19 patients, 42% were found to be Se deficient and as the severity of disease increased, Se plasma levels decreased [160]. These patients also experienced additional nutritional deficiencies. COVID-19 patients compared to healthy controls in India, Iran and Russia had significantly lower plasma Se levels [161,162,163]. A greater rate of low plasma Se levels (<70 ng/mL) was found in COVID-19 patients (43%) compared to controls in India (20) [161]. Lung damage, as assessed by computer tomography, was inversely associated with Se levels in Russia [163].
COVID-19 patients may also experience increases in oxidative stress and increases in Se-related markers and lower Se levels have been documented in these patients. Moghaddam al. [164] observed an association between markers of Se status and COVID-19 outcomes from COVID-19 patients in Germany. Serum Se and SELENOP concentrations were lower in COVID-19 patients compared to a reference European population. A comparison of patients that survived compared to those who died from COVID-19 showed that the deceased had a significantly greater deficiency of serum Se and SELENOP concentrations than those who survived. In addition, those who died had significantly lower serum Se, SELENOP levels, and GPX compared with patients who survived. A study in Belgium using a convenience sample of patients hospitalized with severe COVID-19 pneumonia observed statistically lower GSH levels and higher GPX levels compared with reference intervals among other results showing elevated markers of oxidative stress and lower antioxidant status [165]. Recently, Polonikov [166] hypothesized that GSH deficiency plays a major role in augmenting SARS-CoV-2 oxidative damage, which leads to greater disease progression and mortality. This viewpoint was based on data showing lower GSH and higher ROS levels in COVID-19 patients with mild disease and increasing severity that included higher viral load with GSH deficiency [166] and work completed by Hurwitz et al. [167] that demonstrated improvement in dyspnea with high dose oral and IV GSH in two patients with underlying conditions who tested positive for COVID-19. These conclusions were based on very small samples and therefore require additional larger clinical studies to replicate the findings and eventual intervention studies. The evidence presented above suggests that Se availability contributes to resisting SARS-CoV-2 infection, corresponding with studies that show adequate levels of Se status maintains an appropriate immune response to viral infection [6,134,136].
There are no known published Se supplementation clinical trials in the context of COVID-19 at this time and one study is currently listed on clincaltrials.gov that will examine the efficacy of Se (selenious acid infusion also known as sodium selenite) for the treatment of moderately-ill, severely ill, and critically ill COVID-19 patients (Identifier: NCT04869579). Sodium selenite supplementation has been proposed for the prevention of COVID-19 infections and severe disease [149,168]. Sodium selenite is easily available, short-term toxicity is marginal and may cross the blood-brain barrier [149]. This chemical form may oxidize thiol groups located in the virus protein disulfide isomerase, which would interfere with its ability to infiltrate the cell membrane and produce an infection [168]. TXNRD activity increases quickly after supplementation with sodium selenite in cancer cell lines and critically ill patients [169,170] and has demonstrated reduced ROS production and viral-induced cell apoptosis in cell culture studies [171]. A common feature of COVID-19 is thrombotic complications and altered platelet function is believed to affect the sequelae of this infection [172]. Sodium selenite has also been shown to have an anti-aggregating effect through its reduction of thromboxane A2 formation, an important factor in blood platelet activation and formation [173]. The effectiveness of sodium selenite for the prevention and management of COVID-19 should be tested immediately as the COVID-19 pandemic continues to persist and threaten the health of individuals globally, thus necessitating rapidly accessible treatment strategies.
Since Se has pronounced therapeutic potential for the treatment of viral infections and other conditions such as cancer, Se nanomedicine has received a lot of attention. Se nanoparticles are known to have low toxicity with marked and selective cytotoxic effects with small quantities [174]. Additionally, Se nanoparticles have high effectiveness in the inhibition of oxidative damage [175,176,177]. Recently published data show that Se nanoparticles activate programmed cell death in target cancer tissue through calcium (Ca)2+ signaling pathways [178]. Immune cells also require calcium flux to generate oxidative stress [174]. Through chemical methods, Se nanoparticles may be produced with Se sources that include sodium selenite, selenious acid, and sodium selenosulfate [174]. Due to the developing relationship between Se and COVID-19, Se nanomedicine is being suggested as a tool in the fight against SARS-CoV-2 [179]. Currently, there are tremendous prospects of using nanomedicine in ARDS for the prevention, diagnosis, and treatment, which may have applicability for COVID-19 [180]. Jin et al. [181] discovered that an organic Se compound known as Ebselen, and a promising antioxidant drug, could inhibit SARS-CoV-2 by penetrating the cell membrane and displaying antiviral activity. Ebselen is known to have anti-inflammatory activity, mimic GPX activity, and should be considered for clinical studies [181,182].
Unlike other trace elements that act as cofactors, selenium is covalently bound to organic molecules. Most of the beneficial effects of selenium is due to its incorporation in the form of selenocysteine into an essential group of proteins that are called selenoproteins. Selenocysteine is the 21st proteinogenic amino acid and is encoded by an UGA codon which is normally the signal for termination of protein synthesis [15,16,17,18,19,20,21,22,23]. Selenocysteine is a structural and functional analog of cysteine in which a selenium atom replaces sulfur to confer an enhanced catalytic activity. Amongst the twenty-five selenoprotein genes identified to date, several have important cellular functions in antioxidant defense, cell signaling and redox homeostasis [24]. Within the well characterized selenoproteins we find the following sub-families: Glutathione peroxidase (GPX1–GPX4 and GPX6) that reduce hydrogen and lipid peroxides [25], thioredoxin reductases (TXNRD1–TXNRD3) which are essentials in the homeostasis of thiol systems [26,27,28,29], methionine sulfoxide reductase (MSRB1) [30] and selenoproteins located in the endoplasmic reticulum (DIO2, SELENOF, SELENOK, SELENOM, SELENON, SELENOS and SELENOT) exhibit important functions in protein folding and in the endoplasmic reticulum stress response [31,32,33]. The other half of the selenoproteome remains without a, yet, defined function. Selenoproteins are present in many organelles or cellular compartments, with a specific tissue distribution and sensitivity to selenium level changes. Selenoproteins are therefore important components of antioxidant defense systems maintaining redox homeostasis, which also include catalase (CAT), superoxide dismutase (SOD), glutathione (GSH), vitamin E, carotenoids, and ascorbic acid.
Reactive oxygen species (ROS) are produced during viral infections with both beneficial and deleterious consequences for the cell (Figure 1). The viruses associated with ROS production are human immunodeficiency virus (HIV), hepatitis B virus (HBV), hepatitis C virus (HCV), Epstein-Barr virus (EBV), herpes simplex virus type 1 (HSV-1), vesicular stomatitis virus (VSV), respiratory syncytial virus (RSV), human T cell leukaemia virus type 1 (HTLV-1) and influenza viruses [34]. The mechanisms of ROS generation by the various viruses are diverse, but in several cases the host antioxidant defense enzymes, and especially members of the selenoproteome, are targeted.
2.1. ROS and Oxidative Stress
The term “reactive oxygen species” (ROS) refers to series of side-products derived from molecular oxygen (O2) generated during mitochondrial oxidative phosphorylation in every respiring cells (Figure 1). ROS can also arise from exogenous sources including drugs, xenobiotics, metals, radiation, smocking and infection [35]. ROS consist of radical and non-radical oxygen species formed by the partial reduction of molecular oxygen. They include superoxide anion radical (O2•−), hydrogen peroxide (H2O2), and hydroxyl radical (HO•). At low concentration, ROS are also essential molecules in physiological processes such as cell signaling, proliferation, tumor suppression, and maintenance of the immune system. Oxidative stress arises when an imbalance between ROS and the cellular antioxidant defense system occurs (Figure 1). This could be due to an increase in ROS levels or a decrease in the cellular antioxidant capacity. Oxidative stress leads to direct or indirect ROS-mediated damage of nucleic acids, proteins, and lipids, and this phenomenon has been implicated in many pathological conditions including carcinogenesis [36], neurodegeneration [37,38], atherosclerosis, diabetes [39], and aging [40].
The production of ROS can be assessed indirectly either by using redox-sensitive dyes that are oxidized by ROS into quantifiable fluorescent products, such as 20,70-dichlorodihydrofluorescein diacetate (DCFHDA) or by quantification of cellular oxidation products such as oxidized DNA (8-hydroxydeoxyguanosine), lipids (malondialdehyde, F2-isoprostane, 7-ketocholesterol, and 7-hydroxycholesterol), proteins (carbonyl, 4-hydroxynonenal or glycated oxidation products). Many enzymatic assays are also available to evaluate the antioxidant function of the organisms [41].
2.2. ROS Function in Immunity and Cell Signaling
ROS have an important role in host defense and immunity [42]. The most characterized example is the mechanism by which phagocytic cells produce large amounts of ROS to eliminate a wide variety of pathogens without altering the host cell viability. The nicotinamide adenine dinucleotide phosphate (NADPH) oxidase enzyme complex of phagocytic cells (PHOX) produces superoxide anion radical in the phagocytic vacuole via the transfer of one electron from NADPH to molecular oxygen [41]. The conventional idea is that this (O2•−) molecule dismutates to form H2O2 and other ROS by further chemical or enzymatic reactions [43,44]. Indeed, the myeloperoxidase (MPO) that is an abundant protein released from the granules into the vacuole can further process H2O2 into HOCl. While the mechanism by which ROS can neutralize the invading micro-organisms in the phagosome is still a matter of debate, the production of HOCl by MPO seems to have a predominant role [43,44].
In addition to microbicidal activity, ROS also act as signaling mediators during cell death/apoptosis but also in processes that control cellular proliferation and differentiation. The family of NADPH oxidases (NOX) and Dual Oxidases (DUOX), referred to as NOX/DUOX, are homologs to PHOX and expressed in a variety of tissues, including colon, kidney, thyroid gland, testis, salivary glands, airways and lymphoid organs. A clear role for cytoplasmic ROS generated by NOX2 as well as DUOX1 has been shown in T cell receptor signaling as well as downstream activation and differentiation of T cells [45,46,47,48]. ROS production by mitochondrial complex III is required for antigen-induced T cell activation and production of interleukin-2 which is the cytokine essential for T cell proliferation [49].
2.3. ROS and Viral Infection
Viral infection is often accompanied by alteration of intracellular redox state of the host cell [34,41,50,51,52,53,54,55,56,57,58,59,60] (Figure 1). Viruses are known to induce ROS-generating enzymes, including NOX/DUOX and xanthine oxidase (XO) and to disturb antioxidant defenses. XO is implicated in the catabolism of purine nucleic bases by producing H2O2. Increased of NOX/DUOX and XO activities were observed both in vitro and in vivo during viral infection [41]. Infection by the HIV is associated with decreased levels of GSH and an increased production of ROS [61,62,63]. The latter can be caused directly by virus and/or by the inflammatory response of the host. The viral TAT protein increases intracellular ROS levels by inhibiting the antioxidant enzyme manganese superoxide dismutase MnSOD [64]. In chronic hepatitis C, direct interaction of core protein with mitochondria is an important cause of the oxidative stress [57]. The increase of ROS production has been well documented during HIV, HBV, HCV, EBV, HSV-1, VSV, RSV, HTLV-1 and Influenza viral infections [34]. With HIV-1, ROS were found to stimulate viral replication with the nuclear transcription factor NF-kB, which is necessary for viral replication, being activated by oxidative stress in vitro [54,57,65].
3.3. Role of Thioredoxin Reductase in Antioxidant Defense, Redox Homeostasis and Redox Signaling
The two major reductive systems in mammalian cells are the thioredoxin (Txn) and GSH pathways. The Txn system is completely dependent on selenium as the three thioredoxin reductases (TXNRD1–TXNRD3) are selenoproteins with the selenocysteine residue at the penultimate position of the C-terminal end of the protein [26,28]. TXNRD1 and TXNRD2 are ubiquitously present in the cytoplasm and mitochondria, respectively, while TXNRD3 expression is restricted to specific tissues. The primary substrates of TXNRD1 and TXNRD2 are Txn1 and Txn2, respectively, Txn2 being localized in the mitochondria. TXNRDs catalyze the NADPH-dependent reduction of oxidized thioredoxin (Figure 2B). The Txns catalyze the reduction of protein disulfides such as in ribonucleotide reductase, peroxiredoxins (PRX), MSRB1, protein disulfide-isomerase (PDI), and are therefore critical for DNA synthesis, the defense against oxidative stress and disulfide formation within the endoplasmic reticulum [20]. Peroxiredoxins are able to reduce H2O2, organic hydroperoxides and peroxynitrite in order to protect cellular components from oxidative damage. However, the existence of multiple peroxide-removing enzymes such as catalase, GPX and PRX indicates that these peroxidases are not simply used in oxidant defense [91]. During inflammation, high levels of peroxides are produced by phagocytes to kill microorganisms. It has been well established that PRXs play cytoprotective antioxidant role in inflammation. Recently, it has been proposed that PRXs may play key roles in innate immunity and inflammation [91]. It becomes clear that, in addition to fighting oxidative stress, PRXs are important modulators of peroxide signaling. In addition to Txn, TXNRDs can reduce other small molecules containing sulfur, selenium, or oxidized semiquinone and therefore participate in many other cellular processes [20,26,28,92], Figure 2B.
4.1. Coxsackie Virus
The coxsackie virus is a nonenveloped, linear, positive-sense single-stranded RNA virus that belongs to the family of Picornaviridae (Group IV), genus Enterovirus. These enteroviruses, which also include poliovirus and echovirus, are among the most common and important human pathogens [100,101]. Coxsackie viruses are divided into group A (23 serotypes) and group B (six serotypes) viruses. In general, coxsackie viruses from group A infect the skin and mucous membranes, while viruses from group B infect the heart, pleura, pancreas, and liver [100].
In the early 1930s an endemic cardiomyopathy termed Keshan disease was first described in Heilongjiang province, Northeast China. This disease mainly affects infants, children and women in childbearing age [66]. It is characterized by cardiac enlargement, congestive heart failure, pulmonary edema and death. Keshan disease spread in another 12 provinces across China between the 1940s and 1960s. Approximately eight million people lived in the affected areas during that period of time, and thousands of people died of Keshan disease every year from this pathology. It is only in the 1970s and even the early 1980s, that the selenium contents in soil, water, food, and human body fluids were found extremely deficient in the areas affected by Keshan disease as compared with adjacent provinces [102]. Selenium fertilizer was applied to the soil in order to increase its content in the food [66]. In addition, selenium supplementation of the diet was also given to the people of these areas. The result was the complete eradication of this disease in these provinces of China [103]. However, several features of the Keshan disease, especially the annual or seasonal fluctuation in the incidence of the disease, did not wholly fit with a selenium deficiency. It appears that this disease has a dual etiology, i.e., selenium deficiency and an infectious cofactor, namely the coxsackie virus B [103,104,105,106].
Animal models were used to understand the relationship between host selenium nutritional status and coxsackie virus infection [53,93,94,96,97,98,99,107,108,109,110,111,112]. Coxsackie virus B3 (CVB3) infection of mice can cause myocarditis, similar to that found in human populations afflicted with Keshan disease. Interestingly, as illustrated in Figure 3 the work from Beck and co-authors showed that a non-virulent stain of CVB3 (designated CVB3/0) that do not lead to myocarditis, although replicating, is able to evolve in a virulent strain when inoculated in selenium deficient mice [98,99,109,110,111]. Remarkably, this is also true when Gpx1 knockout mice were infected with the benign strain CVB3/0. The sequencing of the viral genomic RNA isolated from selenium deficient and Gpx1-/- mice demonstrated that a viral genome change had occurred during the infection and replication of the virus as compared to the viral genome replicated in selenium adequate animals, resulting in a highly pathogenic virus [108]. Out of the ten-nucleotide positions that were reported to co-vary with cardio-virulence in CVB3 strains, six reverted to the virulent genotype in virus isolated in Se-deficient mice, and seven in Gpx1-/- mice. Interestingly, a similar finding was also reported with the deficiency of another essential antioxidant, namely Vitamin E [93,94].
These experiments performed in animal models demonstrate that the host nutritional status, and particularly its antioxidant defense system is an important virulence factor, which can greatly contribute to the evolution of benign viral genomes into more virulent viruses. However, the molecular mechanism involved in this process remains to be elucidated.
4.2. Influenza Virus (Orthomyxoviridae)
Influenza viruses are enveloped, linear, negative-sense single-stranded RNA viruses belonging to the Orthomyxoviridae family (Group IV). There are four genus of this family: A, B, C and Thogotovirus, but only three influenza viruses are infectious for humans (A, B and C) [113]. The viral genome consists of eight segmented single-stranded RNA segments (seven for influenza C virus) encoding between 9 to 12 proteins, including hemagglutinin (HA) and neuraminidase (NA) surface glycoproteins, three ribonucleic acid (vRNA) polymerase subunits (vRNP: PA, PB1, PB2), non-structural protein (NS1), and matrix proteins M1 and M2 [113].
Various subtypes of the most common influenza A viruses are classified based on the diversity in the structure of HA and NA proteins. Influenza viruses can be divided into 16 different HA and NA combinations. Influenza A and B viruses cause epidemics, whereas influenza C virus tends to cause infections with less severe symptoms [113]. According to the World Health Organization (WHO), the seasonal epidemics result every year in 3 to 5 million cases of severe illness and in 250 to 500 thousands deaths worldwide (https://www.who.int/influenza/en/). People at highest risk for mortality are the elderly and individuals with chronic diseases of the lung and heart. However, safe and effective vaccines are available but often do not perfectly match the circulating subtypes or become ineffective due to viral antigenic drift [113]. It is therefore necessary to engineer new vaccines and revaccinate people at risk every year.
The patients infected with influenza virus display a marked increase in DNA, lipid and protein oxidation products in blood plasma and urine [41,114,115,116]. Models of mice and cell lines infected with influenza viruses also show an enhanced production of ROS together with an imbalance of antioxidant defense [117,118,119,120]. These models are relevant to study the changes in redox homeostasis induced by the influenza virus.
The work from Beck’s laboratory extended this novel concept that host nutritional status (especially selenium deficiency) is an important virulence factor in a viral family other than enteroviruses, as shown in Figure 4 [95,121,122,123,124]. Indeed, a rapid change in the pathogenicity of the virus in selenium deficient host has been also reported for influenza virus similarly to what was found for coxsackie virus. As shown in Figure 4, mice were fed with a diet either deficient or adequate in selenium for 4 weeks. Then, influenza A/Bangkok/1/79 (H3N2), a strain that induces mild pneumonitis in normal mice, was inoculated to both groups of mice. Interestingly, at all-time points post-infection a clear difference in pathology was observed between the two groups of mice [95,121,122,123,124]. The virus was much more virulent in selenium deficient mice, although with a similar virus titer than the selenium adequate mice. In addition, the sequencing of the HA, NA and M genes of viruses isolated from selenium-adequate and selenium-deficient mice demonstrated a strong impact of selenium status on virus mutation.
It appears that the selenium deficiency of the host promotes rapid genomic evolution of the virus in HA and NA genes as compared with selenium adequate animals [53,95,122,123,124,125]. Strikingly, these mutations are not stochastic as they were identical in three independent mice fed in selenium deficient diet. In comparison, very few mutations were detected in animals fed with adequate selenium diet. These data further confirm the impact of selenium status of the host in viral genome evolution.
4.3. Human Immunodeficiency Virus (HIV)
The human immunodeficiency virus (HIV) is an enveloped, linear, positive-sense single-stranded RNA virus that belongs to the family of Retroviridae (Group VI), genus Lentivirus. Two types of HIV have been characterized: HIV-1 and HIV-2 [126]. Given that HIV-1 is more virulent and more infective than HIV-2, HIV-1 has spread worldwide while HIV-2 is mostly confined to West Africa [127]. HIV is the etiologic agent of acquired immunodeficiency syndrome (AIDS) and is responsible for a weakened immune system as it infects immune cells [126]. HIV affects more than 35 million people worldwide and causes the death of about 1.5 million patients per year (http://www.who.int/hiv/en/). HIV infection is now considered as a chronic disease that requires intensive treatment and can present a variable clinical course. No vaccine is available until now, but an effective medication in decreasing the viral load and increasing the number of CD4 T-lymphocytes has been developed and is referred to highly active antiretroviral therapy (HAART) [128]. This treatment consists in the combination of three or more drugs that target different aspects of HIV replication [129].
HIV genome is highly compact and contains three genes encoding viral structural proteins (gag, pol and env), two genes for essential regulatory elements (tat and rev) and at least four genes encoding accessory regulatory proteins (nef, vpr, vpu and vif). As in any retrovirus, the RNA viral genome is reverse-transcribed in dsDNA that is then integrated in the host genome by the viral integrase. HIV-1 infects immune cells that harbor the CD4 receptor and a co-receptor belonging to the chemokine receptor family (CCR5 and CXCR4) [126]. Therefore, cells infected by HIV-1 are CD4 T-lymphocytes, monocytes, macrophages and dendritic cells. The replication but also the latency of the virus is extremely variable from one cell type to another.
Lentiviruses are characterized by a long incubation period after the primo infection that is highly variable from one patient to another. During this time, humans infected with HIV are under chronic oxidative stress. The redox status of the patient is strongly disturbed in HIV infected patients as revealed by the decrease of antioxidant defense (selenium, ascorbic acid, alpha-tocopherol, carotenoids, superoxide dismutase, glutathione, and glutathione peroxidase) and the increase in ROS production (hydroperoxides, malondialdehyde, and clastogenic factors) [130]. The altered redox status seems to contribute to HIV pathogenesis in several ways. In vitro, increasing oxidative stress enhances the replication of HIV through the activation of NF-kB. Several mechanisms have been reported to explain the cellular enhancement of ROS production in HIV infection. Most of them imply the following viral proteins: Gp120, Tat, Nef, Vpr, and Retrotranscriptase (RT), as reviewed in [50]. A dramatic consequence of this chronic oxidative stress is the fatal decrease in the number of CD4 T-cells by apoptosis, and ultimately a failure of the immune system leading to death.
The nutritional deficiencies of the HIV-infected patient can affect the responsive capacity of the immune system and the progression to AIDS. Selenium is nowadays understood as an essential micronutrient for antioxidant defense and also immune function [131,132]. HIV infection simultaneously increases the demand for micronutrients and causes their loss which leads to a deficiency that can be compensated by micronutrient supplementation [133,134,135]. Low selenium levels are associated with a lower number of CD4 T-cells, faster progression of AIDS, and 20% increase in the risk of death [133,136]. However, little has been done in term of intervention studies by selenium supplementation or at the cellular and molecular levels to establish the link between selenium, selenoprotein and HIV infection. For example, selenium supplementation is only effective in slowing HIV progression for a subgroup of patients, for which serum selenium levels, CD4 count and viral load were improving in contrast to selenium non-responders or placebo group [137,138,139]. However, the cellular and molecular mechanism for this unequal response remains elusive. Although efficient at controlling viral load and restoring immune function, HIV antiretroviral therapies, especially the protease and reverse transcriptase inhibitors, have been shown to induce oxidative stress [50,140]. Interestingly, a long time treatment (more than 2 years) with antiretroviral therapy improves selenium levels as compared with HIV-infected patients not receiving the treatment [141].
The field awaits further investigations to understand the role of selenium and selenoproteins during HIV infection at the molecular level. The only in vitro data available reported a modification of the pattern of selenoprotein expression in response to HIV infection in lymphocytes [142] but these experiments were performed before the complete characterization of the selenoproteome. The impact of selenium status on viral genome mutations and in particular the shift to more virulent viruses has not yet been tested for HIV as it has been done for coxsackie and influenza.
4.4. Hepatitis C Virus (HCV)
The hepatitis C virus (HCV) is an enveloped, linear, positive-sense single-stranded RNA virus that belongs to the family of Flaviviridae (Groupe IV), genus Hepacivirus. Nowadays, about 3% of the world’s population is infected with HCV, which represents approximately 170 million people. Although HCV replication occurs in hepatocytes, the virus also propagates in immune cells. In 80% of the patients with acute hepatitis C, the disease evolves to chronic hepatitis, with 2% developing liver cirrhosis and 1–5% developing liver cancer [143,144]. Many characteristics of oxidative stress have been reported during chronic hepatitis C, including a decrease in GSH, increase in MDA, HNE and caspase activity [145,146]. Zinc and selenium deficiencies increase the risk of chronicity and malignancy [147]. In addition, there is a high prevalence of HCV coinfection in HIV infected patients. The genome of around 9600 nucleotides encodes a unique polyprotein which is co- and post-translationally cleaved into 10 structural and non-structural proteins.
The infection by HCV is another well-documented example of virus-induced generation of ROS. The nucleocapsid protein of HCV, and to a lesser extent NS3, NS5A, E1, E2 and NS4B, are involved in generating oxidative stress in the liver [51,148,149,150,151]. In parallel, the plasma levels of selenium together with erythrocyte GPX activities were significantly lower in HCV-infected patients than in healthy controls. An inverse correlation of selenium levels with viral load was also observed [152]. Interestingly, in HCV and HIV co-infected patients, an even lower serum selenium concentration was measured than in HIV-infected patients [153]. Endoplasmic reticulum stress and unfolded protein response are induced by HCV gene expression [154]. A selenoprotein involved in these mechanisms, SELENOM, has been reported to be upregulated in human hepatocellular carcinoma (HCC) cell lines and liver biopsies of patients with HCV-related cirrhosis [155]. Whether this is true for other endoplasmic reticulum located selenoproteins remains to be investigated.
4.5. Other Viruses
The Hepatitis B virus is an enveloped virus with a circular and partially double-stranded DNA that belongs to the Hepadnaviridae family (Group VII). HBV includes several viruses that infect liver cells and cause hepatitis in humans and animals. In the viral genome, the large negative stranded DNA encodes the envelope, core and non-structural proteins, the DNA polymerase and an oncogenic transactivator [156,157]. The synthesis of the short strand is completed by cellular DNA polymerases after infection. There are 8 HBV strains, from A to H that differ from their geographic repartition [156,157]. Worldwide, between 2 and 8% of the population is infected by HBV but in most of the cases being asymptomatic. An acute HBV infection is however characterized by yellow eyes and skin, severe fatigue, vomiting and abdominal pain. In less than 5% of the cases, the infected people could develop a chronic infection which can further lead to a cirrhosis (in 20% of the cases) [156,157]. Several studies showed an association link between plasma selenium levels and progression of HBV infection [158,159,160]. For example, the selenium level is not correlated with the responsiveness to interferon treatment [161] but an elevated plasma selenium concentration is associated with a low level of transaminases [161]. Theses hepatic enzymes are implicated in amino acid catabolism, and their release in the plasma is linked to hepatocellular damage. In intervention studies, selenium supplementation decreased cancer incidence in HBV infected patients [162], but when the supplementation was stopped, the incidence became similar to control patients. Finally, in vitro, when hepatic cell lines were grown with different selenium concentration, lower viral proteins, viral transcripts and viral genomic DNA were detected with high selenium culture conditions [161].
The Porcine Circovirus 2 (PCV2) is a non-enveloped virus with a circular single-stranded DNA genome which belong to the Circoviridae family (Group II) [163]. Two strains exist, type 1 and type 2, but only type 2 causes a disease in swine, namely the Postweaning Multisystemic Wasting Syndrome (PMWS), a dramatic disease for pig-production industry. The severity of this syndrome is thought to highly dependent on intrinsic factor such as the status of the immune system. It is one of the smallest virus characterized so far, encoding only a capsid protein and two necessary proteins for viral replication [163]. It has been shown that selenomethionine supplementation in cell culture inhibits viral replication [164,165,166,167,168]. Furthermore, addition of H2O2 or ochratoxin A that induced oxidative stress enhanced viral replication. This effect was prevented by selenium supplementation [164,165,166,167,168] or by selenoproteins SELENOS and GPX1 [164,165,166,167,168]. It appears that this mechanism involved the autophagy pathway [164,165,166,167,168]. Finally, in infected mice, selenium supplementation was able to decrease histological lesions by reducing inflammation [164,165,166,167,168].
5.1. 1998: First Example of a Viral Selenoprotein Encoded in Molluscum Contagiosum Virus Genome
Molluscum contagiosum is a viral infection that affects the skin and is caused by the dermatotropic poxvirus molluscum contagiosum virus (MCV) [237,238]. Unlike smallpox and human monkeypox diseases, MCV is nonlethal, mostly common in children and young adults and present worldwide [237,238]. However, MCV causes severe skin infections in immunosuppressed adults [237,238]. A typical feature is the apparition of single or multiple papules on the skin, which may persist for a few years. Most cases resolve in six to nine months without specific treatments [237,238]. Such a prolonged infection implies that MCV successfully manipulates the host environment. In 1998, the analysis of the MCV genome sequence predicted the presence of a candidate selenoprotein, homologous to mammalian GPX, with 75% amino acid sequence identity with human GPX1 [175], see Figure 5A,B. This viral GPX protein is encoded by MC066L gene that presents every features of a selenoprotein gene, i.e., an in-frame UGA codon, a stop codon different from an UGA (in this case UAG), and a SECIS element in the 3’UTR of the mRNA (Figure 5A). The absence of homologs of this gene in vaccinia and variola viruses suggests that the GPX-like gene was acquired by the MCV after the divergence of the Molluscipoxvirus and Orthopoxvirus genera. The expression of this predicted selenoprotein was tested experimentally in mammalian cells. Indeed, when a plasmid containing the MC066L gene was transfected in human skin cell lines, many evidences supported the insertion of a selenocysteine residue at the UGA codon in the full-length protein, the functionality of the SECIS elements and the cellular antioxidant activity of the MC066L protein [175,239]. Remarkably, this viral selenoprotein has been shown to be protective for human keratinocytes against cytotoxic effects of UV-irradiation and hydrogen peroxides [175,239], suggesting an important function for the virus in defending itself against environmental stress and inflammation. How and when this selenoprotein is expressed in the context of viral infection remains poorly investigated. The first transcription map of the MCV genome was provided by the transcriptome sequencing (RNA-seq) of the RNAs synthesized in abortively infected cultured cells and human skin lesions [240]. These next generation sequencing experiments showed that MC066L mRNA was only detected in cutaneous lesions, but not in MRC-5, Huh7.5.1 and Vero cells infected in vitro by the MCV virus isolated from these same skin lesions.
5.2. 2007: A Second Example of an Encoded Viral Selenoprotein in Fowlpox Virus Genome
Almost ten years later, another example of an encoded viral selenoprotein was reported in fowlpox viral genome [176], see Figure 5C,D. This was due to the increasing number of viral genome sequenced but also to the development of novel bioinformatic tools dedicated to the discovery of selenoprotein genes in newly sequenced genomes [79,80,81]. In this viral genome, a coding region homolog to the mammalian GPX4 gene was found, with an in-frame UGA codon, and a predicted SECIS element downstream of the UGA codon but this time within the open reading frame instead of being in the 3’UTR. This finding represented a great opportunity to investigate whether this putative viral SECIS or a canonical SECIS could function within the open reading frame. The authors demonstrated that mammalian cell lines supported the expression of selenoproteins with in-frame SECIS element from both viral and mammalian origin. This fowlpox SECIS element was the second example of a functional viral SECIS element with a structure being identical to the mammalian SECIS. Interestingly, in an evolutionary related virus, the canarypox virus (CPV), this gene has evolved in a Cys-containing GPX4 with a fossil SECIS element still present in the coding region (Figure 5C,D). The potential of this fossil SECIS to trigger recoding of an UGA codon in selenocysteine has not been investigated. It appears that there was a recent mutation of the selenocysteine into cysteine codon in canarypox virus, as it has happened multiple times during evolution of the selenoproteomes in Eukarya, Bacteria and Archaea [79,80]. Note that cysteine is encoded by UGC and UGU codons, and that a single mutation is able to change a selenocysteine to cysteine codon and vice-versa. The presence of a fossil SECIS element indicates that the GPX4 selenoprotein gene was first acquired from the host and recently converted to the Cys form.
The fact that at least two selenoproteins are encoded by viral genomes suggests that these proteins provide a substantial advantage for viruses. Similar to molluscum congatiosum GPX1, the fowlpox GPX4 may provide survival benefits for the virus. These two proteins are, so far, the only proven examples of genetically encoded viral selenoproteins.
5.3. Putative Selenoproteins in Other Viral Genomes
These two examples of selenoprotein gene snatching from eukaryotic genomes in the viral genomes of fowlpox and molluscum contagiosum viruses lead to the careful investigation for further examples of selenoprotein genes sequences with viral genomes. The first analysis searched for GPX modules within viral genomes where an in-frame UGA codon would be in an amino acid environment close to the catalytic site sequence of eukaryotic GPXs. Several candidates with sequence identities greater than 25% were found in the genomes of HIV-1, HIV-2, HCV, coxsackie virus B3 and measles viruses [183]. Despite these in silico data that GPX-related features are present in a number of RNA viruses, no RNA structure similar to the SECIS element can be evidenced. Additionally, no biochemical data demonstrated the expression of viral selenoproteins in any of these cases. It is possible that viruses have developed somewhat unique mechanisms for Sec insertion, as suggested in [195], but this remains purely hypothetical in the absence of further experimental proofs.
Perhaps, the most advanced study concerns a putative GPX protein coded in the third reading frame of the envelope (Env) gene of HIV-1 [241]. Indeed, it contains the typical catalytic triad selenocysteine (U), Glutamine (Q) and Tryptophan (W) and this putative HIV-GPX protein has been predicted to adopt the overall GPX fold, as deduced from computerized calculations [233]. In addition, it appears that the HIV-GPX gene is conserved in laboratory strains of HIV-1, as well as in long-term non-progressor isolates, but most of HIV isolates from patients with progressive disease presented deleterious mutations (mostly premature stop codons). In order to grasp the cellular function of this putative HIV-GPX in mammalian cells, the corresponding coding sequence has been fused to a mammalian SECIS element and transfected in mammalian cells [234]. The expression of the HIV-GPX seems to have an anti-apoptotic activity, by conferring cytoprotection against exogenous or endogenous ROS. Indeed, several viral proteins are known to induce apoptosis via redox-sensitive effects during HIV-1 viral cycle. Therefore, the presence of a HIV-GPX could be pertinent in the long-term non-progressor patients. Note that these experiments were performed before the emergence of the HAART.
Another putative viral selenoprotein gene has been reported in the -1 reading frame of the NS4 region of Japanese encephalitis virus (JEV). JEV belongs to the Flaviviridae family, which also includes dengue fever virus (DENV), yellow fever virus (YFV) and West Nile virus (WNV). The gene named NS4-fs encodes a potential 104 amino acid sequence with three predicted selenocysteine residues, i.e., three in frame UGA codons [191]. This putative selenoprotein displays 30.3% identity and 45.8% similarity with an aligned family of ferredoxin with cysteine instead of selenocysteine. Noteworthy, these three UGA codons are highly conserved, as they are present in all of the 15 full genomic JEV sequences analyzed. A 3D structure of the protein has been modeled [191] where the selenocysteine residues are proposed to maintain the conformation of the [Fe2S2] cluster center. Interestingly, ferredoxin usually acts as an electron transfer agent in biological redox reactions, and this may somehow be important for JEV infection or replication. Again, in this example, neither SECIS elements were found nor any biochemical evidence of selenoprotein expression was provided.
During viral infections, there are many ways that the host metabolism could be affected, leading to a dysregulation of redox homeostasis. The viral pathogens induce oxidative stress via the increase generation of ROS and the alteration of cellular ROS scavenging systems. As part of antioxidant defense, selenoproteins, such as GPXs, TXNRDs and those located in the ER, play an important role in controlling oxidative stress. Selenium deficiency creates a weakening of the defense against infectious diseases by reducing selenoprotein expression. However, nutritional status of the host can also lead to viral genome mutations from a benign or mildly pathogenic virus to a highly virulent one under oxidative stress that could further spread in hosts with adequate selenium intake.
Further studies on selenium can be found here:
Green Tea Extract
Proposed Mechanism: Contains catechins, which have antiviral properties and are thought to inhibit viral replication.
EGCG was found to inhibit Porcine reproductive and respiratory syndrome virus (PRRSV) infection irrespective of whether it was administered before or after infection; a concentration of 125 μM was enough to completely inhibit the infectivity of viral cells (Ge et al., 2018). In Hepatitis C virus (HCV) infection, EGCG was found out to inhibit the infection by attaching to the target cell and preventing the spread of the infection to different cells (Calland et al., 2012). It was also proposed that EGCG inhibits the entry of the ZIKA virus by interacting with the lipid bilayer. A significant point to be noted is that an in vivo study showed that ECGC can cross the placental barrier and spread to the brain, eyes and heart of the foetus, hence making its administration effective in pregnant women and possibly the foetus also (Chu et al., 2006). EGCG was found to inhibit not only the intracellular chikungunya virus replication but also the extracellular infection in the pre and post stages of viral infection (Lu et al., 2017). EGCG is expected to inhibit the intermediate stages of the influenza virus cycle apart from the known mechanism of affecting the virus attachment by inhibiting hemagglutination activity (Song et al., 2005). EGCG has also been found effective against HIV-1 and inhibits viral replication by acting at various stages. It blocks interaction of gp120 with CD4 by interfering with reverse transcriptase (Sodagari et al., 2016). A report suggested that EGCG inhibits the production of p24 antigen on isolated CD4 receptor cells, macrophages and CD4±T cells depending on its dose (Nance et al., 2009). Another report suggested that even at concentrations obtained by consumption of green tea, EGCG is seen effective in inhibiting gp120-CD4 attachment (Williamson et al., 2006).
As evident from the mechanisms of action of EGCG in various viruses, it is a wide spectrum antiviral agent with its mechanism differing from infection to infection. The difference in the antiviral activity can be attributed to the number of hydroxyl groups present on the benzene ring and galloyl group, together with the pyrogallol group which is responsible for exhibiting diverse mechanisms (Xu et al., 2017).
Like EGCG, antiviral properties of theaflavin polyphenols and their derivatives have also been explored in several viral diseases. In a study on HSV-1, among all the theaflavins tested individually, TF1, TF2, and TF3 showed strong inhibition of the viral lytic cycle with TF3 being the most potent. It was shown that there was more than 99% inhibition of the infectivity of viral molecules when they were treated with TF3 at 50 μM for 1 h, thus proving its prophylactic antiviral activity (de Oliveira et al., 2015). In another study, TF2 was found to exhibit its anti-inflammatory effects in vivo by suppressing the levels of COX-2, TNF-A, 1CAM-1, and NFkB mRNA. Also, the radical quenching ability of TF3 was observed with the induction of mitochondria hyperpolarization which indicated activation of apoptotic signaling (Gosslau et al., 2011). A study on the influenza virus also showed the antiviral activity of TFs via neuraminidase inhibition; the activity of TF3 was better than other derivatives and almost comparable to the control oseltamivir carboxylate (Zu et al., 2012). TF3 was also seen to prevent the virus from adsorbing into the MDCK cells hence inhibiting the hemagglutinin of the virus (Nakayama et al., 1993). TF2B was found to be the most potent among all the other tea polyphenols in the inhibition of HIV at a concentration of 1 μM and a selectivity index greater than 200. The number of galloyl groups on the TF had a direct relation on its activity and it is estimated that these molecules interact with the gp41 six-helix bundle to prevent viral entry into the host cell (Liu et al., 2005). At a relatively higher concentration, TFs were also found to inhibit reverse transcriptase in HIV (Jie et al., 2011). TFs were found to have best in-silico antiviral activity among 2080 small molecules against caliciviruses. The study also proposed that hydroxyl groups in TFs are more essential in exhibiting the activity over the galloyl groups (Ohba et al., 2017). A study reported that TFs show activity directly on the HCV viral particles to inhibit their binding to the surface of the receptor. It highlighted that TF3 exhibited better anti-HCV activity than TF1 and TF2 (Chowdhury et al., 2018).
2.1. GTC Inhibits HBV
Infection with hepatitis viruses is the main cause of hepatitis in the world. There are five types of hepatitis viruses: types A, B, C, D and E. Types B and C are the major cause of chronic liver diseases, such as liver fibrosis, cirrhosis and hepatocellular carcinoma. HBV is a serious threat to international human public health, as hundreds of millions of people are infected. Despite vaccination programs, the possibility of and potential for outbreaks and epidemic spread cannot be excluded. Unfortunately, the most commonly used medications or therapies for HBV have success rates that are dependent on viral genotype and suffer from several limiting side effects [17]. Therefore, finding and identifying more effective therapies without side effects is of great importance.
HBV is a member of the Hepadnavirus family with a 3.2-kb genome of partially double-stranded DNA. In 2008, we reported the anti-HBV activity of GTCs in HepG2-N10, a stable cell line expressing HBV antigens [9]. We found that the expression of HBV antigen and the synthesis of extracellular HBV DNA, intracellular replicative intermediates, and cDNA and HBV mRNA were inhibited when HepG2-N10 cells were treated with various concentrations of green tea extracts. Other research groups have also documented similar results; for example, EGCG had strong effects on the expression of two HBV antigens and could prevent the production of HBV genomic DNA [18,19]. Using HepG2.117, an inducible HBV-replicating cell line, He et al. observed that EGCG significantly inhibited the RNA synthesis of intracellular replicative intermediates [20]. However, in HepG2.117 cells, the synthesis of HBV pregenome RNA, precore mRNA and HBeAg was not affected [20]. To clarify the molecular mechanism of the anti-HBV effects of EGCG, we used florescence quenching and affinity binding experiments [21]. We found that among five different GTCs, EGCG showed the strongest inhibition of HBV antigen expression. The associated mechanism may involve EGCG acting as an antagonist of the farnesoid X receptor alpha (FXRα) and the interaction between EGCG and FXRα down regulating the transcriptional activities of the HBV EnhII/core promoter [21].
In 2014, Huang et al. found that different genotypes of HBV could be inhibited by EGCG in immortalized human primary hepatocytes and two constructed cell lines, DMSO-differentiated HuS-E/2 cells and HA-NTCP-expressing Huh7 cells (NTCP is the receptor of HBV) [22]. Furthermore, in the membrane, clathrin-dependent endocytosis of NTCP was induced and directed to protein degradation pathways by EGCG. However, EGCG did not change HBV structures or the expression of genes involved in HBV entry. Recent evidence indicates that during infection, host cells can trigger autophagy, a lysosomal degradation mechanism that is important for cell survival. The results of Zhong and co-workers indicated that to combat the incomplete autophagy induced by HBV, EGCG can create a microenvironment that is detrimental to HBV replication by altering lysosomal acidification [23].
2.2. Effect of GTCs on Herpes Simplex Virus
Herpes simplex is a viral skin disease caused by infection with herpes simplex virus type 1 (HSV-1) or herpes simplex virus type 2 (HSV-2). Both HSV-1 and HSV-2 are enveloped viruses possessing a relatively large double-stranded, linear DNA genome and belong to the Herpesvirus family. HSV-1 is commonly spread through mouth-to-mouth contact and causes cold sores and genital herpes. HSV-2 is usually spread by sexual contact and generally causes only genital herpes [68]. The anti-HSV activity of GTCs was observed by Lyu et al. in 2005 [11]. The authors found that among the 18 tested flavonoids, EC, ECG, EGC and EGCG showed strong anti-HSV activity [11]. A subsequent investigation demonstrated that EGCG showed stronger activity against HSV than the other GTCs tested and made infectious clinical isolates of HSV-1 and HSV-2 lose their infection ability [24]. The data also showed that inactivation of the virus occurred because of a direct destructive effect of EGCG on the HSV-1 virions [24]. Another study from this research group showed that digallate dimers of EGCG could inactivate HSV and could be developed into more effective antiviral drugs against HSV [25]. The results of case studies from Zhao and co-workers suggested that a topical formulation containing EGCG-stearate in 100% glycerin could prevent and treat HSV-induced symptoms [26]. Palmitoyl-EGCG (p-EGCG), a modified EGCG, increased the effectiveness of EGCG as an anti-HSV agent in HSV-infected Vero cells [27]. An interesting study exploring the reason for the broad-spectrum antiviral activity of EGCG demonstrated that EGCG competitively interacted with virion surface proteins to inhibit the attachment of HSV-1 to heparan sulfate [28]. Moreover, in this study, EGCG showed its broad-spectrum antiviral activities on many other viruses, including HCV, IAV, murine cytomegalovirus (mCMV), vaccinia virus (VACV), vesicular stomatitis virus (VSV), reovirus, and adenovirus. This activity was possibly related to a common mechanism: the interaction between the virus and heparan sulfate or sialic acid was inhibited [28].
2.3. Effect of GTCs on the EBV
The EBV is another member of the herpes family and infects humans [69,70]. EBV is one of causes of many types of malignant tumors and certain autoimmune diseases. It produces lytic infections in most epithelial cells and latent infections in most B-cells (from which it reactivates periodically producing a reactivating infection) [71]. Some researchers investigated the anti-EBV effects of EGCG using different cell models. They found that EGCG not only suppressed the synthesis of some lytic proteins of EBV but also inhibited the lytic infection by downregulating the transcription of immediate-early genes or reducing the DNA binding potency of nuclear antigen [29,30]. Additionally, Liu et al. explored the molecular mechanisms of the anti-EBV activity of EGCG in spontaneous lytic infection in vitro [31]. The results showed that the anti-EBV lytic infection mechanisms of EGCG could be associated with inhibition of the MEK/ERK1/2 and PI3-K/Akt signaling pathways [31].
2.4. Effect of GTCs on Adenovirus
Adenovirus is an icosahedral non-enveloped DNA virus approximately 60–90 nm in diameter. Adenovirus infection can cause cold-like symptoms, sore throat, bronchitis, pneumonia and pink eye. People can contract an adenovirus infection at any age. Weber et al. found that EGCG at micromolar concentrations reduced the virus titers of adenovirus in two cell infection models and inactivated purified adenovirions [32]. The results from Colpitts and co-workers showed that EGCG inhibited the attachment of adenovirus by interacting with virion surface proteins [28].
3. Inhibitory Effects of GTCs on RNA Virus
3.1. GTC Inhibits HIV
In 1994, Chang et al. reported for the first time the anti-HIV activities of polyphenolic catechins from Chinese green tea [34]. The authors isolated EGCG, EC and ECG from Camellia sinensis and demonstrated their potential as new inhibitors of HIV reverse transcriptase (RT). HIV, the pathogen of AIDS, was identified by Barré-Sinoussi and Luc Montagnier in 1983 [72]. There are two types of HIV: HIV-1 and HIV-2. HIV-1 was initially discovered and is the predominant virus, while HIV-2 is less transmissible. There are around 1~2 million cases of HIV-2 infection with unique geographical and age distribution. According to the World Health Organization (WHO), since the beginning of the HIV epidemic, approximately 70 million people have been infected with HIV and more than 35 million people have died of various diseases caused by HIV. At the end of 2015, there were approximately 36.7 million HIV carriers globally [73]. Therefore, to cure AIDS, studying novel drugs and seeking new treatments is very important. Before major inroads had been made in anti HIV therapy and vaccine in the last few years [74,75], more than a dozen research groups paid efforts into the fields of anti-HIV effects of tea catechins, mainly anti-HIV-1.
EGCG is an inhibitor of HIV reverse transcriptase. Chang et al. have reported that three catechins, namely, EC, ECG and EGCG, demonstrate strong inhibitory action against HIVRT [34]. Kinetic analysis showed that the tested catechins were competitive inhibitors of the template-primer and noncompetitive inhibitors of dTTP [34]. In human peripheral blood mononuclear cells (PBMCs), EGCG acting as an inhibitor of HIVRT could decrease the expression of the HIV p24 antigen, which subsequently resulted in inhibition of RT activity [8]. A report from Li et al. revealed that both HIV-1 and HIV-2 infection were suppressed by lower physiological concentrations of EGCG [35].
EGCG inhibits HIV entry into target cells. In 2002, Yamaguchi et al. reported that EGCG has a destructive effect on viral particles of HIV-1, causing a decrease in the ability of virions to infect cells and inhibiting viral attachment to cellular surfaces [36]. The HIV envelope protein gp41 plays a key role in the fusion between the viral envelope and the plasma membranes of target cells. The assembly of six-helix bundles (6HB) of gp41 is an indispensable step during fusion; subsequently, these 6HB predominantly govern the conformation of the fusion-active core. By blocking the 6HB formation of gp41, EGCG inhibits the membrane fusion of HIV-1 mediated by the envelope glycoprotein and thus blocks HIV-1 from entering cells [37]. The gp120 protein is another envelope glycoprotein of HIV that is essential for viral entry into cells, as it acts on the attachment to CD4 receptors on specific T-cell surfaces. EGCG can block gp120-CD4 binding through the preferential formation of the EGCG-CD4 complex, which results in an extreme reduction in the binding strength of gp120-CD4 [38]. Nuclear magnetic resonance spectroscopy, flow cytometry and molecular modeling from Williamson’s research group showed that the binding between EGCG and CD4 strongly reduced the formation of the gp120/CD4 complex. A binding site for EGCG was found on CD4 in the D1 domain, which is the gp120 binding pocket [39]. Using PBMCs, CD4 (+) T cells, and macrophages isolated from blood, Nance et al. reported that at physiological concentrations, EGCG weakened the binding activity of gp120 to CD4 by a dozen-fold [40].
EGCG attenuates neuronal damage mediated by HIV infection. HIV-associated dementia (HAD), previously referred to as AIDS dementia complex (ADC), is a condition caused by the action of HIV-1 infection on the central nervous system and leads to patients having difficulties with memory and learning. HAD is related to the activation of proinflammatory cytokines and neuropathology involving gp120 and Tat (a transactivating regulatory protein) of HIV. EGCG can mitigate neuron injury in the presence of IFN-gamma both in vitro and in vivo [41]. Using an HIV-1 Tat transgenic mouse model, Rrapo et al. demonstrated that EGCG could decrease the number of Tat-expressing astrocytes, mildly reduce activated microgliosis and enhance neuron survival [42]. In rodent cerebral cortical and hippocampal neuronal cultures, EGCG can function in the signaling pathway composed of brain-derived neurotrophic factor (BDNF) and its precursor proBDNF. Furthermore, EGCG balanced the increase in proapoptotic proBDNF and decrease in mature BDNF mediated by Tat [76].
Semen-derived enhancer of virus infection (SEVI) is a fibrillar structure and an important HIV-1 sexual infection factor that captures virions and guides them to their targets. EGCG can inhibit SEVI activity by complex formation and degradation [43,77]. Hartjen et al. confirmed and extended the findings of Hauber et al. using 47 fresh human semen samples [44]. They also observed a semen-independent inhibition of HIV-infectivity that the inhibition rate of HIV infectivity reached 88.5% post-treatment with 0.4 mM EGCG in the absence of semen. The findings above suggested that EGCG may be an alternative drug for preventing the sexual transmission of HIV.
3.2. EGCG Inhibits HCV
HCV is another major cause of chronic liver disease and can causes both acute and chronic infections. Timely antiviral therapy can cure more than 95% of persons with HCV infection, but access to diagnosis and treatment is currently low. According to the recommendations of the WHO, all patients with hepatitis C should be treated with sofosbuvir, daclatasvir and the sofosbuvir/ledipasvir combination based on direct-acting antivirals (DAA), except for a few specific groups of people in whom interferon-based regimens can still be used [78]. Although related researches are ongoing, there is currently no available effective vaccine.
HCV is a Flaviviridae family member with a positive-sense single-stranded RNA genome and a small enveloped virus. In recent years, researchers have studied the anti-HCV activities of EGCG. Several independent research groups reported that EGCG was a potent inhibitor of the HCV entry pathway but had no effect on viral replication, viral RNA synthesis or virion secretion [10,46]. Moreover, Ciesek et al. found that EGCG can stop cell-to-cell transmission when the extracellular route of ingestion is blocked by overlaid agarose or incubated with neutralizing antibodies [10,45]. Besides EGCG, Calland’s group demonstrated that ECG and EGC had anti-HCV activities at an early step of the viral life cycle [10]. Chen et al. found EGCG not only suppressed HCV entry, but also inhibit viral RNA replication [47]. Recently, a new mechanism for the anti-HCV activity of GTCs was reported by Calland and co-workers [48]. Their results indicated that after EGCG treatment, an observed bulge was found on the viral particle and this kind of structural alteration did not result in destruction or aggregation of virons. [48]. The authors also identified delphinidin, a natural molecule with a similar structure to EGCG, as a new inhibitor of HCV infection that prevents HCV entry [48].
Using HCV JFH-1 infectious systems, Lin et al. reported that HCV replication was inhibited significantly by epicatechin isomers. They revealed that the mechanism of the anti-HCV activity of the epicatechin isomers most likely operates through the downregulation of COX-2 [49]. Moreover, these isomers suppressed inflammation by downregulating the expression of inflammatory factors such as tumor necrosis factor-alpha, interleukin-1 beta, inducible nitrite oxide synthase and COX-2 in viral protein-expressing hepatoma Huh-7 cells [49].Another interesting study evaluated the effect of oral doses of EGCG on cirrhotic patients with HCV and found that 400 mg of EGCG was safe and well tolerated; however, the cirrhosis of these patients did not obviously improve. Although the estimate was from limited samples, it provided guidance to researchers for further experiments or observations [79]. Results from Colpitts’s group demonstrated that EGCG interacted with surface proteins of dozens kind of virions, including HCV, and this interaction led to a failure of membrane fusion mediated by heparan sulfate- or sialic acid-containing glycans [28].
3.3. Inhibitory Effects of GTCs on Influenza Virus
Influenza virus includes the pathogens of flu outbreak in birds and many mammals including human, pig, horse, whales, seals, bat and so on. There are four types of influenza virus: A, B, C and D, which are categorized according to the antigenicity of the nucleocapsid protein. Influenza A virus (IAV) is a member of the family of Orthomyxoviridae and has a segmented single-stranded, negative-sense RNA genome. IAV is the main virus of the flu pandemic because of its high mutation rate. As early as 1949, Green et al. reported the antiviral activity of tea extracts against influenza virus [50]. The first serious discussion of the effects of EGCG against influenza A and B viruses was demonstrated in Madin-Darby canine kidney (MDCK) cells by Nakayama’s research group in 1993 [51]. They found that the infection of both IAV and influenza B virus (IBV) was inhibited by EGCG. Moreover, EGCG exerted agglutination effects on virions and prevented the virus from absorbing onto the cell surface [51]. Imanishi et al. further revealed that the anti-IV activity of green tea extracts that included EGCG possibly arose from its inhibitory effects on the acidification of endosomes and lysosomes [52].
To determine the relationship between the structure and activity of different GTCs, Song et al. evaluated their capabilities to inhibit the replication of viruses. They found that EGCG exerted more inhibitory effects than ECG and EGC on the activity of both viral neuraminidase and viral genomic RNA synthesis, suggesting the 3-galloyl group of the catechin skeleton was more important for antiviral activity than the 5’-OH in the trihydroxy benzyl moiety at the 2-position [53,54]. Some researchers explored the inhibitory effects of EGCG analogs, derivatives, and formulations on influenza virus [55,56,80]. Furuta et al. used deoxy-EGCG, a simplified analog of EGCG prepared by directly introducing a ketone group at C3, to show that the hydroxyl substituents on the A-ring of EGCG played a minor role in the anti-influenza virus activity [80]. Two interesting studies by Oxford’s group showed that QR-435, a natural extract from green tea, blocked transmission of IAV H3N2 and provided prophylaxis against H3N2. More interestingly, wearing masks containing QR-435 was able to prevent H3N2 infection [55,56]. Fatty acid monoester derivatives of EGCG, especially those with long alkyl chains, exhibited a sharply increased antiviral effect against IAV compared to natural EGCG [57]. The inhibitory effects of different nutrient mixtures of natural EGCG on influenza virus have also been demonstrated by different investigators [58,81,82]. Some researchers contributed to clinical trials of EGCG as an IAV restriction factor [59]. Moreover, one research group investigated the relationship between influenza virus infection and gargling tea catechin extract and demonstrated that GTCs significantly lowered the rate of influenza infection in 124 elderly residents aged more than 65 years [59]. In another randomized, double-blinded trial of 200 healthcare workers, consumption of capsules including GTCs for 5 months had a protective effect against IAV virus compared with the placebo group [60].
3.4. Effect of GTC on Some Arboviruses
Arbovirus refers to a group of viruses that are transmitted by insects, mostly commonly mosquitoes and ticks, sucking blood for nutrients or development [83]. The most common signs of infection with arboviruses are fever, headache, and general malaise. Severe patients present signs of encephalitis and hemorrhagic fever [84]. The infections caused by different arboviruses, including DENV, West Nile virus (WNV), Japanese encephalitis virus (JEV), tick-borne encephalitis virus (TBEV), and new outbreaks of ZIKV and CHIKV in Latin America, are now becoming serious health threats, especially in tropical and subtropical countries [83].
Recently, molecular docking methods proposed that EGCG can dock in the same binding domain of different E proteins from DENV, JEV and TBEV [14]. Furthermore, the amino acid residues associated with the DENV2 E protein were identified. CHIKV, which is an alphavirus, is transmitted by mosquitoes and causes chikungunya fever in humans. Weber et al. demonstrated the inhibitory effects of EGCG on CHIKV in vitro using a CHIKV-m Cherry-490 infection model. Moreover, they found that EGCG played a useful role in blocking CHIKV from entering the target cells and had a minor effect on CHIKV replication [15]. ZIKV, a member of the Flaviviridae family, has a single-stranded RNA genome and is spread by mosquitoes. Since its outbreak in Brazil in 2015, ZIKV has spread rapidly on a global scale [85]. EGCG showed antiviral activities against ZIKV according to a study from Carneiro et al. in 2015 [16]. Using Vero E6 cells and two strains of ZIKV, namely, ZIKVBR and MR766, they provided evidence for the vital anti-ZIKV function of EGCG. The associated mechanism was also explored. EGCG did not regulate the expression of cell receptors related to viral invasion. Therefore, it is speculated that there was a direct interaction between EGCG and the viral envelope, followed by destruction of the structure of ZIKV virions.
3.5. Effect of GTCs on Human T-cell Lymphotropic Virus-1
Adult T-cell leukemia (ATL) is an aggressive T-cell malignancy caused by human T-cell leukemia virus type I (HTLV-1) infection. In the 30 years since HTLV-1 was discovered, of ATL tend to yield poor results, and little progress has been made in the cure rate [86]. Therefore, searching for new agents that target specific molecules and application of anti-HIV drugs needs to be encouraged [87]. Two groups independently contributed to the discovery of EGCG as an HTLV-1 restriction molecule and found that its inhibitory effect was achieved by suppressing HTLV-I pX and Tax gene expression [61,62].
3.6. Effect of GTCs on Rotaviruses and Enteroviruses
Rotaviruses and enteroviruses are viruses that can cause a series of intestinal symptoms. Enterovirus 71 (EV71) is the major pathogen of hand, foot and mouth disease. In addition, EV71 can lead to diarrhea, rashes and severe neurological disease. EV71 has done great harm to preschool children’s health in both developing and underdeveloped countries. As early as 1991, ECGC from green tea was reported to inhibit rotaviruses and enteroviruses in cultured rhesus monkey kidney cells by interfering with virus adsorption [63]. Ho et al. provided the first evidence for an anti-enterovirus function of GTCs [64]. The authors found that the production of infectious progeny virus of EV71 was reduced by 95% post-treatment with EGCG and gallocatechin gallate (GCG) and suggested that the inhibitory effects were related to the reduced reactive oxygen species (ROS) generation upon EGCG treatment [64].
3.7. Effect of GTCs on EBOV
The Ebola virus (EBOV) is among the most feared viruses and can cause Ebola hemorrhagic fever, a highly fatal disease. The recent WHO statistics showed that the 2014–2016 EBOV outbreak in West Africa had a high fatality rate of 28~75% [88]. Reid et al. identified a host chaperon protein, HSPS5, as an important target for therapies against EBOV infection and found that EGCG, as an inhibitor of HSPS5, reduced the production of new viruses via its action on HSPS5 [65].
3.8. Effect of GTCs on Viruses Infecting Other Animals
Fish and other animals not only are good dietary sources of protein, but also have great natural value and can provide substantial economic and scientific benefits. However, diseases caused by fish virus infections can effect heavy economic losses and influence the development of fish farming. EGCG has been suggested to be able to inhibit infections of some novirhabdo viruses, such as hemorrhagic septicemia virus (VHSV), hematopoietic necrosis virus (IHNV) and spring viremia carpvirus (SVCV), specifically because of its ability as a low-molecular-weight inhibitor of serine protease inhibitor gene transcripts 1 (SERPINe1) [66]. In 2016, the activity of GTCs against grass carp reovirus (GCRV) was demonstrated for the first time by Wang et al. [67]. The results showed that adhesion of GCRV virions to target cells was inhibited in a dose-dependent manner when the cells were treated with EGCG and crude extracts of green tea. It was inferred that the blocking effect of EGCG on GCRV attachment was due to the binding potential of GCRV particles to the laminin receptor (LamR) [67]. Porcine reproductive and respiratory syndrome (PRRS), an endemic pig disease, has caused great losses in the pig industry globally. Its pathogen is a peculiar and highly infectious virus, porcine reproductive and respiratory syndrome virus (PRRSV). Pregnant sows and piglets infected with PRRSV can develop severe reproductive deficiencies and respiratory symptoms, respectively. Using MARC-145 cells, Zhao et al. explored the anti-PRRSV activities of EGCG and EGCG palmitate in vitro. The authors found that the inhibitory effects of both EGCG and its palmitate on PRRSV were dose dependent and that EGCG palmitate showed a much stronger antiviral activity as a pretreatment compound than EGCG [13]. The activities of EGCG and EGCG-loaded chitosan microcapsules against murine norovirus were reported by Gomez-Mascaraque in 2016. The results demonstrated that the encapsulated EGCG was significantly more active than free EGCG [89].